The June 2011 MEDPAC report provides important information about private insurance options to cover dual eligibles (persons covered by Medicare and Medicaid) amplifying yesterday’s post on care coordination.
The Medicare Modernization Act of 2003 created a category of Medicare Advantage plans called Dual-Special Needs Plans (D-SNP) that only cover dual eligibles. D-SNP are a subset of Special Needs Plans (SNPs) that are private insurance options for groups with unique and complex health care needs. SNPs have been created to cover Medicare beneficiaries living in a nursing home, or having chronic disabling conditions such as End Stage Renal Disease, HIV, and congestive heart failure. Table 5-2 (p. 128) from the MEDPAC report provides SNP enrollment:
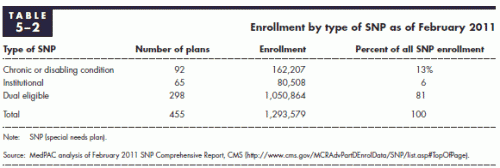
There were around 1.05 million dual eligibles in D-SNP plans in February 2011 (11.4% of all duals), and nearly 1.3 million persons enrolled in all SNPs. SNPs differ from other types of Medicare Advantage plans in several ways (e.g. they must cover part D; you can enroll at any time and not only during open enrollment windows if such a plan is available in an area). Several quick thoughts:
- The problem being addressed is the high cost and potentially non-optimal quality of the care provided to the dual eligibles.
- The goal of proposals to federalize the Medicaid costs of the duals, as well as to move duals into private plans are to incentivize and empower one payer to decrease costs while improving quality for dual eligibles.
- Austin and Aaron have pulled together lots of evidence showing that public payers have done a better job at restraining costs over time than private ones. Most of this literature predates D-SNPs. Studies showing slower cost inflation in Medicare than private insurance were obtained with the dual eligibles (a very expensive group) being cared for by FFS Medicare.
- MEDPAC says that most of the D-SNP plans (p. 128) do not provide fully integrated and coordinated care to the degree believed to be optimal to duals, typically because they do not coordinate Medicaid benefits. Standards and regulation for these plans will expand due to aspects of the Affordable Care Act that will require quality assessments of plans (2012), and a requirement that D-SNPs have state contracts with Medicaid for the coordination of and provision of services (mostly LTC, by 2013).
- There are other types of coordinated activities for dual eligibles described in the MEDPAC report that are implemented outside of the D-SNP approach (PACE, state carve outs, other demonstrations p.124-26 ). Overall, MEDPAC says 2% (p. 124) of dual eligibles are in fully integrated plans. This is not a subset of the D-SNPs but includes other options as well.
- Finally, Austin’s point from last week that lowering spending may not be the appropriate question to ask about whether expanding private insurance options in Medicare is a good one to remember. It would be great to improve quality and reduce costs, but doing both will be hard. The current default for how care is financed for dual eligibles leaves room for improvement on both counts and we need to try and evaluate different options.
