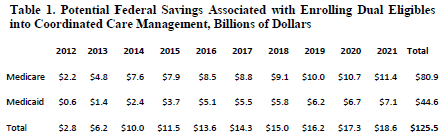Ken Thorpe has a new study funded by AHIP out in white paper form that suggests that moving all dual eligibles (covered by Medicare and Medicaid) into private plans using care coordination could save the federal government and states $125 billion over 10 years. Thorpe notes that CBO projects that combined Medicare and Medicaid spending on the duals will be $3.7 trillion over 10 years by default, owing to their multiple health care needs (over half have 5+ chronic conditions and many reside in nursing homes). The 9 million dual eligibles are among the most sick and vulnerable members of society.
Thorpe proposes defaulting dual eligibles into private plans who will have strong incentive to reduce costs since they would be responsible for all care; similar incentives for Medicare and Medicaid are now reduced owing to the ways they share the cost of caring for the duals. A few details:
- All dual eligibles would be enrolled in a health plan with an opportunity to opt out. All covered Medicaid and Medicare services would be provided through the health plans.
- States can innovate and design their own approaches, but must have an evidence based design.
- Health plans would be responsible for coordinating the multiple needs of their patients, including contracting with other entities such as community health teams (defined in section 3502 of the Affordable Care Act) or medical homes.
The paper includes a rich literature review that suggests costs can be reduced while improving quality, and he includes a simulation of potential 10 year savings if all duals were in private plans: $80.9 billion for Medicare and $44.6 billion for Medicaid, around $35 billion of which would be savings to the states (clearly upper bound estimates):
I have suggested that dual eligible costs should be federalized (essentially making Medicare responsible for their total cost), with the main point being to put one payer in charge of all their care in order to incentivize cost reduction while increasing quality. Thorpe’s idea would achieve the same general goal using private insurance. There are many relevant details to discuss about Thorpe’s proposal (how would premiums for private plans be set?, what are realistic uptake estimates?, etc.), but it is clear that the current approach to caring for the dual eligibles is wanting both in terms of cost and quality. The only question is what changes should be undertaken to better care for them?
Update: There has been lots done on TIE about private v. public plans and cost control and the evidence tilts toward public doing better than private at controlling costs [FAQ and podcast]. Most Dual Eligibles have not been in private Medicare plans, so the balance of the evidence does not include them. However, the special needs plans do cover duals. There was some interesting tweeting yesterday about distribution of dual eligibles in such plans; I will try and track down a linkable source and blog about these issues more over the next week. Finally, by noting in the first sentence of the post that this is a ‘white paper’ that means it has not been subjected to peer review.