As a follow-up to my previous post, a way to help patients make more efficient decisions about their care comes under the rubric of shared decision making (SDM), about which I’ve written before. Emily Lee and Ezekiel Emanuel do so as well in the current issue of NEJM.
A sleeper provision of the Affordable Care Act (ACA) encourages greater use of shared decision making in health care. For many health situations in which there’s not one clearly superior course of treatment, shared decision making can ensure that medical care better aligns with patients’ preferences and values. One way to implement this approach is by using patient decision aids — written materials, videos, or interactive electronic presentations designed to inform patients and their families about care options; each option’s outcomes, including benefits and possible side effects; the health care team’s skills; and costs. Shared decision making has the potential to provide numerous benefits for patients, clinicians, and the health care system, including increased patient knowledge, less anxiety over the care process, improved health outcomes, reductions in unwarranted variation in care and costs, and greater alignment of care with patients’ values. […]
Unfortunately, this ideal is inconsistently realized today. The care patients receive doesn’t always align with their preferences. For example, in a study of more than 1000 office visits in which more than 3500 medical decisions were made, less than 10% of decisions met the minimum standards for informed decision making.1 Similarly, a study showed that only 41% of Medicare patients believed that their treatment reflected their preference for palliative care over more aggressive interventions. […]
Section 3506 of the ACA aims to facilitate shared decision making. Primarily, it funds an independent entity that would develop consensus-based standards and certify patient decision aids for use by federal health programs and other interested parties. In addition, the secretary of health and human services is empowered to fund, through grants or contracts, the development and evaluation of these tools. Decision aids are meant to be evidence-based and inform patients of the risks and benefits of tests and treatments, their relative effectiveness, and their costs. Health care providers will be eligible for grants to implement these tools and to receive training and technical support for shared decision making at new resource centers. The ACA also authorizes the Center for Medicare and Medicaid Innovation to test shared-decision-making models designed to improve patients’ and caregivers’ understanding of medical decisions and assist them in making informed care decisions. For approaches that provide savings or improve quality of care, implementation can be mandated throughout Medicare without additional legislation.
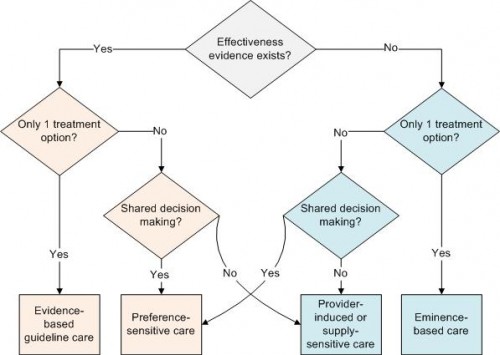
The authors go on to document the demonstrated benefits of SDM to reduce unwanted and unnecessary care. Finally, they make a few suggestions consistent with my own. SDM should be integral to the care provision process. We should pay for it and penalize when it is not used where appropriate. Here’s my chart that indicates the role SDM could and should play, about which more here and here.