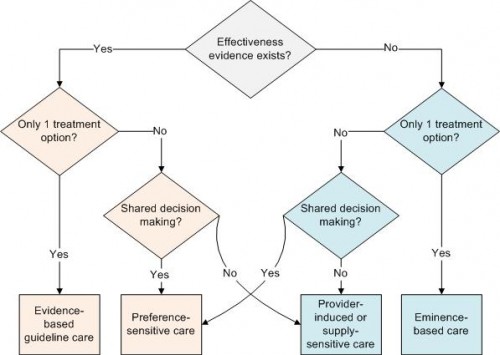
In my latest post on the JAMA Forum I offer a typology of health care that clarifies when various types of cost control are appropriate. The typology is summarized with this chart, which the post explains. (Its structural, though not chromatic, bilateral symmetry reminds me of a butterfly. Could be just me.)
I freely admit the chart and typology are not perfect. It’s pretty hard to simplify health care down to something that can be expressed in a readily-grasped chart and a 1,000-word post. On-and-off, I spent months on this chart, getting feedback from the smart people I acknowledge in my post. The earlier versions were much more complex, and far less clarifying. In the spirit of “all models are wrong, but some are useful,” I assert that this is of some value. Read the post, and let me know if you agree. If not, why not?
By the way (#1), more and more I am disliking the term “cost control” since, in my view, it’s a doubly misunderstood term. People usually use “cost control” when they mean “spending reduction” or “spending growth moderation.” I think the emphasis should be on efficiency, not spending or its growth per se. But we don’t have a nice catch phrase in health policy discourse that unambiguously evokes an efficiency focus. That’s a shame.
The second level of misunderstanding is an ironic one. “Cost control,” with a literal interpretation of what “cost” is, is actually closer to “efficiency enhancement” than some may realize. We should want to maximize health (output) per unit of real resources (input). This is a measure of cost. That is, we should want an increase in efficiency though a reduction in cost at any level of spending, but I think too few people understand this. “Cost control” ends up being an overloaded term to which people yoke whatever collection of ideals for and understandings of health care they harbor. That makes it useless for precise communication. I hope my typology and discussion thereof helps clarify some of the nuances, at least for the six of you who read it. (Come on, spread the word, and make it 12.)
By the way (#2), in response to my “I (partially) quit” post, I was dismayed to hear that some people weren’t paying as close attention to our (mine and Aaron’s) JAMA Forum and AcademyHealth posts as they do to those on TIE. That’s a mistake. Our JAMA and AcademyHealth posts are among our most developed and highest quality posts. They’re worth reading. You’ll find all of TIE’s AcademyHealth posts here. You’ll find all of the JAMA Forum posts here, even those by non-TIE authors. Go read them (or at least those by me and Aaron, though others are good to), staring with my latest.