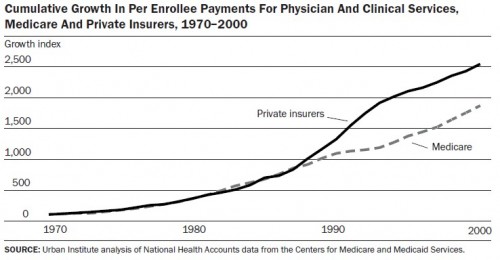
Looks like the very simple analysis I presented in my prior post is consistent with published work, albeit covering a different time period. The following figure appears in Comparing Medicare And Private Insurers: Growth Rates In Spending Over Three Decades, by Cristina Boccuti and Marilyn Moon (Health Affairs, 2003; ungated here).
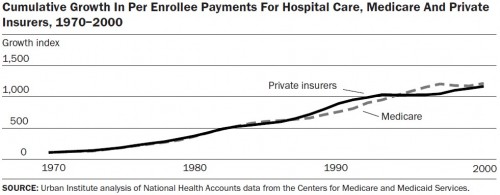
Growth in payments by private insurers for physician services outpaced that of Medicare in the decade of the 1990s. In case you’re wondering, the paper shows Medicare with roughly the same cumulative growth rate as private insurers for hospital payments. See:
Putting all comparable services together, Medicare achieved a lower growth rate in the 1990s than private plans (figure not shown; it’s in the paper). It’s important to note that Medicare may control costs better than private plans on average, there are specific plans in specific markets that outperform Medicare. A competitive bidding system that included both private plans and FFS Medicare would obtain the best of both worlds (where “best” is defined in terms of cost control).