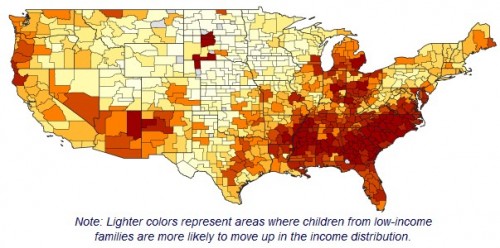
From a new study, which has received considerable attention:
Compare to this, via Bill Gardner:
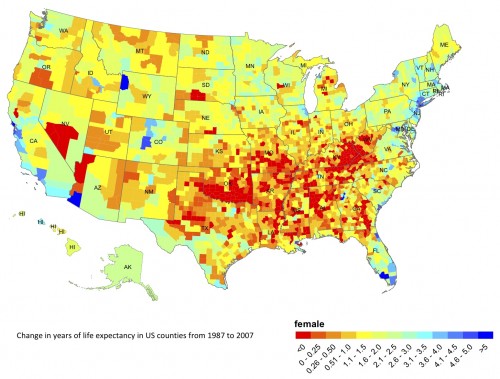
Read the captions and/or follow links for details. Correlation doesn’t imply causation. (And, how correlated are these?) This warrants further study and comment, for which I’m not (at the moment) prepared or qualified. So, blog post for the taking.