If you haven’t read the introduction, go back and read it now. That introductory post also includes links to all the posts in this series on how we can rate the quality of the US health care system. Each of these pieces will discuss another way to look at quality, and how the US compares to comparable countries in that domain.
We wouldn’t have a complete series without some mention of physicians and their practices. They are, after all, an essential component of the health care system. Some measures of their capacity, and their perceptions of quality deserve to be recognized in this series.
For this series, I will be drawing data from The Commonwealth Fund. Specifically, I will be referencing their Survey of Primary Care Physicians in 11 Countries, 2009: Perspectives on Care, Costs, and Experiences. Here are some details:
Mail, phone, and e-mail survey of primary care physicians from February to July 2009 in Australia, Canada, France, Germany, Italy, Netherlands, New Zealand, Norway, Sweden, United Kingdom, and United States
Samples: 1,016 Australia, 1,401 Canada, 502 France, 715 Germany, 844 Italy, 614 Netherlands, 500 New Zealand, 774 Norway, 1,450 Sweden, 1,062 United Kingdom, and 1,442 United States
Core Topics: System views and satisfaction, access to care, managing chronic illness, teams, information technology, measuring practice performance, and financial incentives
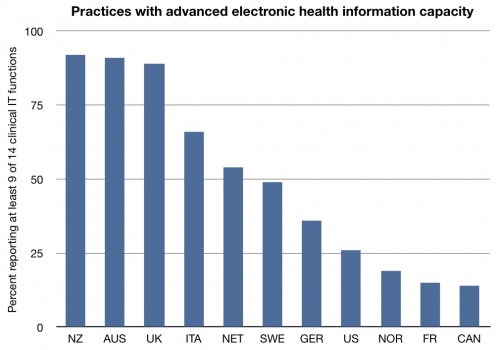
So let’s begin. First up, how well prepared are physician offices with respect to modern technology for quality improvement and practice management?
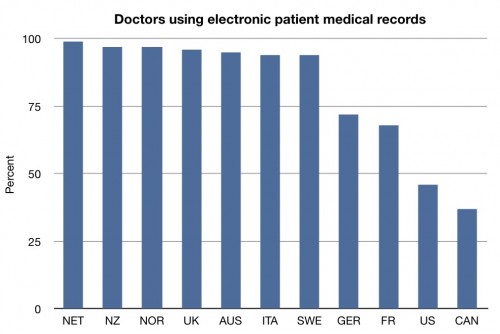
It should come as no surprise to anyone paying attention that the US is surprisingly deficient when it comes to electronic medical records. While I am not convinced of the cost savings of EMRs in all settings, many studies have shown that they increase the potential for quality improvement.
But records are only one part of how technology can be used in practice. The survey also addressed specific tasks. In fact, the survey asked about fourteen specific functions:
electronic medical record; electronic prescribing and ordering of tests; electronic access test results, Rx alerts, clinical notes; computerized system for tracking lab tests, guidelines, alerts to provide patients with test results, preventive/follow-up care reminders; and computerized list of patients by diagnosis, medications, due for tests or preventive care
Here are measures of how many practices reported having at least 9 of these 14 functions:
Still not so good. Very much towards the bottom.
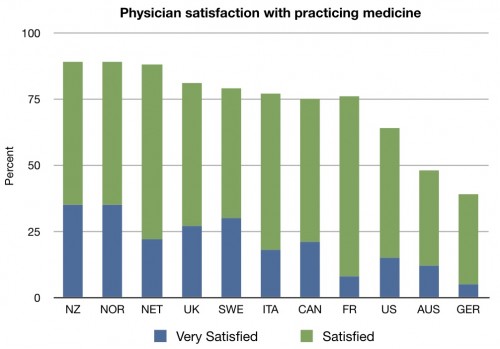
How satisfied are physicians with their practice? It’s not a perfect measure, but it’s an important one:
Given the rhetoric of how much physicians hate reform, you would think doctors were very happy before reform passed. You’d be wrong. With the exception of Austria and Germany, fewer doctors were satisfied with practicing medicine than any other surveyed country.
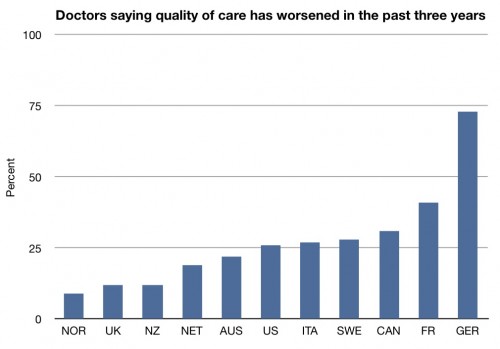
Let’s look at how doctors feel about the quality of care that patients are getting in the system:
Here, the US is more towards the middle. Only about a quarter of physicians in the US think that the quality their patients have been experiencing has worsened in the last three years.
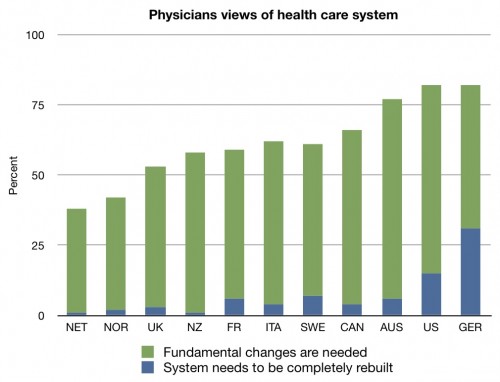
That doesn’t mean that doctors judge the quality of the system to be good, though. That was asked as well:
With the exception of Germany, more US physicians felt that the system needed to be completely rebuilt than physicians in any other country. And the US tied with Germany for last in numbers of physicians who thought the system needed a total reboot or fundamental changes.
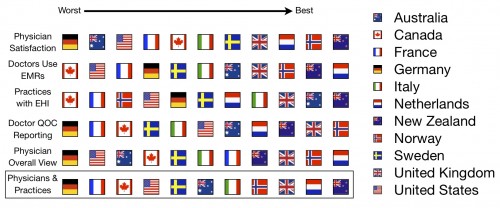
So how do physicians and practices make our system look? We’re pretty deficient in terms of information technology, physicians are unsatisfied with their work, and their views of the quality of patient care and the health care system range from mediocre to terrible. Not a ringing endorsement.
Here’s your sixth scorecard:
And here’s the running total for the series:
A further explanation of these charts can be found here.