This journal is about being a cancer patient during the COVID epidemic. Last week I had a conversation with my doctor that shattered me. I have so much to say! But first, I need to convey what we have learned.
After completing radiation therapy in September, I have steadily regained my health. I am working and writing full-time. I spend an hour or more each day on my yoga mat and exercise bike. My sense of taste has almost wholly returned, so I can cook. Everything has pointed toward a complete recovery, an outcome consistent with the data showing that radiation is usually curative for oropharyngeal cancers caused by human papillomavirus exposure.
Everything, that is, except for two things. First, the pain at the site of my primary tumour has never gone away. Second, I have had a computerized tomography (CT) scan and a positron emission tomography (PET) scan that were consistent with persistent cancer. My clinicians were skeptical of these results because these tests have high false-positive rates, and the evidence shows that radiation usually works. To resolve this uncertainty, I had a surgical biopsy a week ago this Monday.
The pathology report from the biopsy appeared — amazingly quickly — in my electronic health record on Tuesday night. The pathologist found that my tumour had survived radiation and was continuing to grow.
On Thursday, I met with my surgeon. Evidently, the biopsy was sobering news, yet I was calm. When I was first diagnosed last July, I had assumed that I would need surgery. Moreover, I knew that surgery could cause severe morbidity because my tumour was near the root of my tongue. Specifically: I might lose the ability to speak, and I might be feeding permanently through a gastric tube. But in this worst case, I would still have far more than Stephen Hawking did, and I was confident that the procedure, as invasive as it was, would nevertheless leave me with a life I would greatly value. I was ready to do it.

So I went to the meeting assuming that its purpose was to discuss the resection of my throat to cut out the tumours.
But that didn’t happen. Here is the gist of our conversation:
Surgeon: I’ll review your options. First, there is palliative care.
What?
Surgeon: Second, there is medical assistance in dying. [This is legal in Canada.]
Me: That is not an option for religious reasons.
Surgeon: I understand. I mentioned these options first because we do not have much to offer in the way of treatment. I have spoken with Dr. X [my radiation oncologist]. As you know, you can’t tolerate additional radiation. Neither of us thinks that chemotherapy gives you any benefit at this stage. But I will arrange an appointment with Dr. Y [a medical oncologist with whom I had previously discussed chemotherapy] to discuss that further. Now let’s talk about surgery.
I explained to him that I understood that surgery could entail the loss of essential functions. But if it were curative, and I could be with my family and still write and do science, that would be acceptable.
Surgeon: And I would support that view. The problem is that the surgery would also damage your epiglottis, which protects your lungs from infection. You would experience repeated pneumonias, requiring hospitalization, one of which would likely kill you. And for all that, it would only offer you a slight chance — perhaps 10% — of a cure.
Oh.
Surgeon: The last option is to look for a clinical trial of experimental therapy. I know this is difficult to hear, and I would be happy to help you get a second opinion.
Please don’t criticize my surgeon for his direct style. We know each other well, and he knew how much I value his honesty.
How did I feel? Shattered.
By which I mean that I felt the urgent need to pursue a thousand lines of thought — “IS palliative care something to consider?” “How do I convey this news to my brother?” “They keep saying ‘salvage’; how is that different from any other type of medicine?”… — with each new thread interrupting the one that preceded it. And I felt grief. Not (thank you, God) despair, anger, resentment, or even fear. Instead, grief for the impending separation from my wife, children, work, home, future, and even my dog.
Grief, yes, but also confusion. We are all Bayesians now, and we expect each additional data point to move our beliefs, but not move them too much. That’s how things work, > 99% of the time.
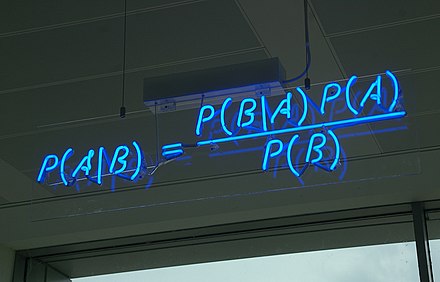
However, there are moments in every life when the data demolish your beliefs and change everything going forward.* You are informed that they have let you go from a job where you had excelled on every evaluation. You watch terrorists knock down skyscrapers with airliners.
What confused me was that I felt great. The night before the meeting, perhaps to prove that I was healthy, I had set a personal record for kilojoules of output during a 45-minute ride on my Peloton bike. And yet my doctor told me that I had 6 to 18 months to live. How could this be?
What’s challenging to hold in your mind is that a tumour is like an epidemic: it grows exponentially. The chart below shows daily new COVID-19 cases in Nepal. On March 20, 2021, was anyone prepared for what would happen in the next month?
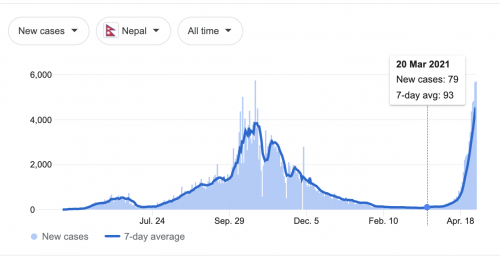
Likewise, a tumour starts off too tiny to matter. Then it doubles, but it is still small. Then it doubles again and again, and sooner rather than later, it kills you. Tracking back through the scans, my tumour seems to double every couple of months.
I haven’t stayed shattered. This is good because it turns out that dying — if that is what I’m doing — entails surprising numbers of meetings and lots of paperwork. It would be incautious to say I have hope, but I have a direction, including a second opinion. Thanks for listening, more later.
*Of course, my experience wasn’t truly inconsistent with Bayes’ theorem, but let’s not get too pedantic here.
