We can debate the importance of life expectancy as a metric of quality in a health care system, but few can deny it’s still worthwhile to examine what kills us. The CDC has released its latest data on Death in the United States, 2010:
- Life expectancy at birth is 78.7 years. Hispanic females have the longest life expectancy (83.8 years) followed by non-Hispanic white females (81.1 years).
- The largest decrease in mortality between the years 2000 and 2010 occurred in the age group under age 25 years (15.8 percent), followed by those aged 65 years and over (13.3 percent).
- States in the southeast region generally have higher death rates than those in other regions of the country.
- In 2010, the five leading causes of death were: heart disease, cancer, chronic lower respiratory diseases, stroke, and accidents. The ranking of conditions varies according to demographics such as age, sex, and race.
- The infant mortality rate reached a record-low level of 6.14 infant deaths per 1,000 live births in 2010.
The most important statistic is the age-adjusted death rate, because the makeup of the US population with respect to age keeps changing. That rate was 746.2 per 100,000 population, a 0.5% decrease from 2009. The CDC attributes much of this to improvements in our care of heart disease, cancer, stroke, and chronic lower respiratory disease.
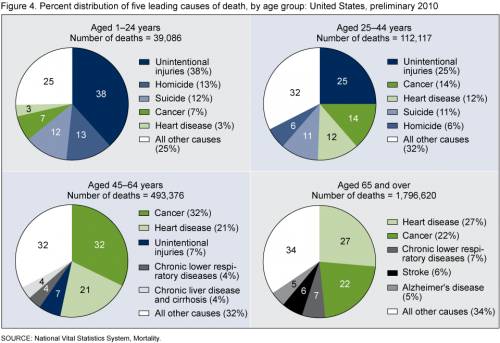
As always, I want to know what affects children. So this figure caught my eye:
That’s the distribution of the five leading causes of death by age group. Yes, if you’re 65 or older, it’s disease that’s gonna get you. But as you get younger, the causes of death leave the strictly medical world. For those less than 25 years of age, the top three causes of death are, in order: accidents, homicide, and suicide. Together, these three categories cause 63% of all deaths.
They’re largely preventable. But they won’t be cured by insurance, by drugs, or by medical technology. As we continue to focus on ways to improve the health care system, we shouldn’t ignore the fact that for children, violence and accidents are – by far – the most likely thing to kill you. Preventing those deaths are important, too.