Medical technology always seems to be advancing. This includes the ways we screen for breast cancer in women. Digital imaging and computer-aided detection have become much more common. The use of magnetic resonance imaging (MRI) and ultrasound has increased as well. All of this is thought to improve our sensitivity in detecting breast cancer. It’s thought that it will allow us to diagnose breast cancer earlier, when more can be done.
Unfortunately, that doesn’t appear to be true.
A just-released paper in the Journal of the National Cancer Institute followed more than 270,000 women who were part of fee-for-service Medicare in two cohorts. The first was comprised of women 66 years of age or older with no history of breast cancer on January 1, 2001. The second was of similar women on January 1, 2008. All women were followed for two years, or until they were diagnosed with breast cancer or died.
The overall use of screening mammography didn’t change much over time. In the earlier cohort, 42% of women were screened, and in the later cohort, 42.6% of women were screened. However, the use of digital mammography increased from 2% to 29.8%. The use of computer aided detection went up from 3.2% to 33.1%. Diagnostic mammography, which would follow a positive screen, went up from 5.3% to 7.1%. Ultrasound use went up from 4.0% to 4.9%, and MRI use went from 0.03% to 0.3%. All of these changes were statistically significant.
However, the rates of cancer detection over the study period barely changed at all. There was no significant difference in the overall rate of breast cancer detected, which was 4.22 per 1000 person years in the earlier cohort and 4.30 per 1000 person years in the later cohort.
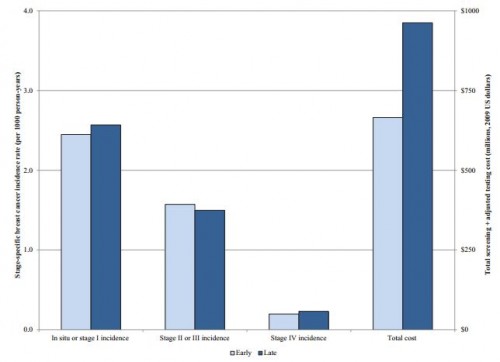
There was also no improvement in the stage at which breast cancer was detected. Early stage breast cancer was diagnosed in 2.45 versus 2.57 per 1000 person years (not significant). But late stage breast cancer was diagnosed similarly, in 0.20 versus 0.23 per 1000 person years (not significant). In fact, there was no improvement at all in the stage at which women were diagnosed or the tumor size at the time of diagnosis.
It’s important to remember that this is the metric on which the advanced technology is sold. It’s supposed to pick up cancer at an earlier stage and when the tumor is smaller. That doesn’t seem to be the case.
It is definitely more expensive, though. The cost of screening mammography per beneficiary went from $44 to $63 (in constant 2009 dollars). The cost per mammogram went from $75 to $101, mostly because of the shift from film to digital technology. The cost of additional imaging and biopsies went from $32 to $43.
The overall screening related costs per beneficiary went up more than 47%. This means that overall breast cancer screening related expenses went from $666 million in 2001-2002 to $962 million in 2008-2009 (constant 2009 dollars).
The best that can be said here is that the shift to digital mammography did not appear to cause any harm. There have been concerns that the increased sensitivity of the technology could lead to more over-diagnosis and significant increases in diagnosis of in-situ cancers that post no immediate threat. That concern did not manifest in this study.
However, the more important point is this: we’re paying a lot more money for no real gain. The ratios of cancer diagnosed at different stages have not improved, nor have the sizes of tumors diagnosed. That is what this “better”, and more expensive technology, was supposed to accomplish.
Nevertheless, Medicare reimburses more for digital mammography than for film mammography. Why? I don’t know. These data certainly don’t make a case for it.
There has been a robust debate for years as to whether we screen too aggressively for breast cancer. As I’ve argued here before, the actual improvements seen from randomized controlled trials don’t support large gains for universal screening, and the harms, and costs, are considerable. It’s worth noting that almost a third of the women receiving screening mammography in both cohorts were 75 years or older. About half of women had at least one comorbid condition that would increase their chance of dying earlier. It’s not clear how much a universal screening program could lengthen the lifespan of such women. It may wind up causing them to undergo more unnecessary procedures.
Even if that debate continues, though, it’s hard to continue to make an argument that using more advanced technology is a good thing if it doesn’t improve measurable outcomes. We waste enough money in health care already. Wasting more won’t help.
