Today in the NEJM, Kelly Kelleher (of Nationwide Children’s Hospital) and I discuss rural US kids with mental health and developmental disorders, and the obstacles to caring for them.
We summarize new data from the Centers for Disease Control about the epidemiology of these problems among rural kids. We also discuss data from the US Department of Agriculture which show that poverty is higher among rural children than urban children and that rural child poverty is higher than it has been since 1993.
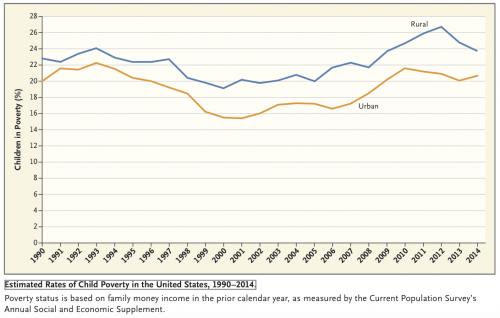
Then we look at the many obstacles to getting services to kids in rural settings, particularly the lack of mental health specialists. It’s a problem in the US and Canada, both of which have large regions with low population densities.
We conclude:
A romantic and pastoral view of the countryside as a place of healing is ingrained in American culture. The increased burden of MBDDs among rural children belies this image, as does the failure of the traditional behavioral and developmental health care system to address rural children’s needs. These problems have received too little attention, because most behavioral and developmental health specialists, researchers, and health policymakers live in cities. The problems of rural children, their families’ crises, and the lack of services have been out of sight and out of mind.
And of course I have to say: please read the whole thing!
Our article was in press before the text of the AHCA was released. Sara Rosenbaum reports that the bill changes Medicaid in several ways.
the House bill essentially eliminates the enhanced funding levels that made possible states’ expansion of Medicaid to their poorest working-age adult residents, something that 31 states and the District of Columbia now have done. Expansion states could face up to a 40-point difference between the federal funding enhancements they expected to receive in 2020 for the expansion population and what they actually would receive under the bill. What is at stake is continued coverage for some 11 million of the more than 16 million people who have gained eligibility since full implementation of the ACA Medicaid expansion.
The proposed changes could harm rural America, and rural American kids specifically, in two ways.
First, many rural families are covered by Medicaid. Losing this coverage will increase the stress on already highly-stressed families. Medicaid funding is also critical to the children’s hospitals that are among the primary places that kids get care for developmental and mental health disorders.
Second, rural Americans are currently experiencing a significant public health crisis involving opiates, amphetamines, and suicide. Parental substance abuse can adversely affect children. The AHCA has a provision that may undermine efforts to address the substance abuse epidemic. Katie Zezima and Chris Ingraham report in the Washington Post that
Beginning in 2020, the plan would eliminate an Affordable Care Act requirement that Medicaid cover basic mental-health and addiction services in states that expanded it, allowing them to decide whether to include those benefits in Medicaid plans.
There are large areas in rural Americas where there are no addiction services. If Medicaid funding shrinks, state administrators will look for places to cut. Eliminating the requirement to fund mental health and addiction services means that funding shortfalls will disproportionately affect kids with mental health and developmental disorders.
