It’s frustrating, becaus whenever I show data on how we don’t do so well in caring for one disease or another, someone inevitably tries to “gotcha!” me by claiming that there’s a good explanation for it, other than the fact that our system is lacking. Today’s excuse seems to be “the prevalence must be the reason”.
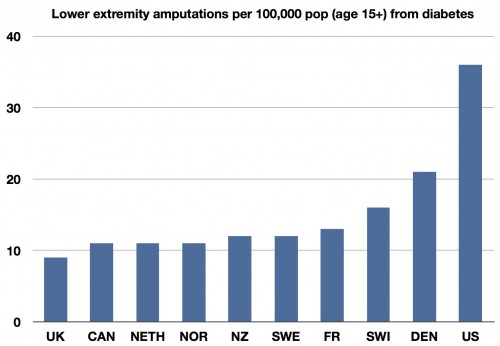
A number of you have emailed me, or commented, that it may be that the reason there are more amputations in the US is because diabetes is much more common here. More people sick = more amputations. So here’s the chart of amputations again:
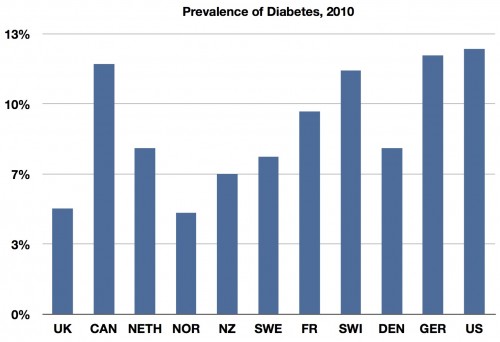
And here’s the prevalence of diabetes in those countries:
Yes, we have a lot of diabetes in the US, but not so much more than everyone else, and they all do better than us. One in particular on the left (which gets a bad rap on “difficulty to get care”) has nearly the same prevalence in diabetes and less than one third the amputations.
Someday, you’ll learn to trust me. Or at least, to trust Occam’s Razor.
UPDATE:
ARGH! 🙂
1) I didn’t have these data “handy”. They take time to take down and chart. But now I’ve done it.
2) Data on Germany were not available for amputations. Go look at the link to the original data I provided.
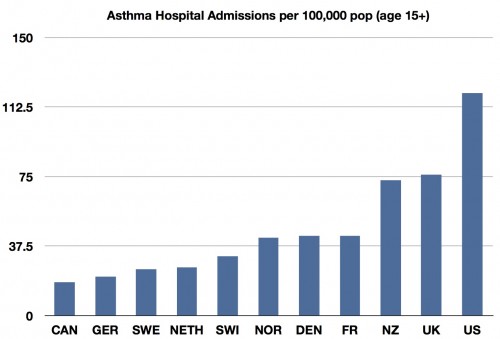
3) Here’s Asthma. First hospital admissions again:
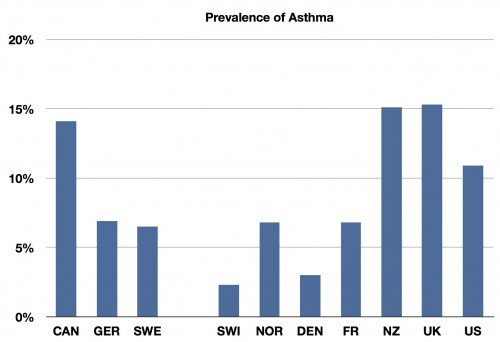
And then prevalence. Data were not available for the Netherlands, and I used England for the UK. Scotland and Ireland were even worse: