America’s Health Insurance Plans (AHIP) is a trade association representing private health insurance companies including those that operate most Medicare Advantage plans. AHIP opposed the Affordable Care Act (ACA), spending heavily on ads that criticized the President and Democrats for supporting cuts in Medicare Advantage payments. These cuts, which Austin and I have shown would fall mostly on plans, not on beneficiaries, were scored by the CBO as worth $136 Billion over 10 years. They are the backbone of the financing for expanding coverage to the uninsured and one of the few real cost control measures in the law.
In the mid-term election the Democrats fared poorly. Many Democratic candidates had difficulty explaining their votes in favor of ACA, particularly to elderly Medicare beneficiaries concerned about Republican and AHIP charges that it will cut their Medicare benefits. On Veterans’ Day, just 8 days after the election, the Obama Administration quietly released a new regulation expanding quality bonuses to Medicare Advantage plans that receive only average quality ratings. Julie Appleby of Kaiser Health News reported a few days later that some analysts interpreted this as a gift to the plans worth about $1.3 billion over 3 years ($5.3 billion over 10 years). Austin and Brad Delong both expressed concern that this could be the beginning of the political unraveling of one of the few cost controls in the ACA.
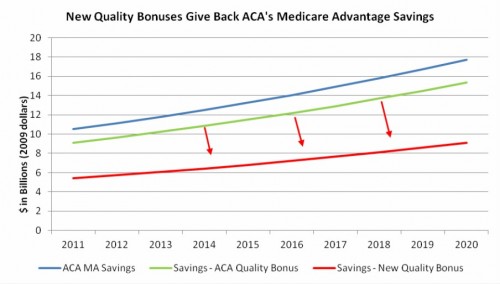
How could a $5.3 billion give-away make a meaningful dent in $136 billion in savings? It couldn’t. But the $5.3 billion figure is probably wrong. A more realistic estimate is almost ten times larger.
The original quality bonus program written into ACA targeted bonuses to plans receiving 4 or 5 “stars”, representing approximately 23% of enrollees according to Brian Biles and Grace Arnold of George Washington University who analyzed the data last April. The new regulation will grant bonuses to plans receiving 3 or more “stars”, representing 84% of enrollees (3.7 times as many). Biles and Arnold estimated the cost of the original bonus program at $1.4 billion per year as long as plans don’t respond to the bonuses by improving their quality ratings. The details of the expanded bonuses have not yet been released, but if we assume the new program will be similar to the old one, we can make a rough calculation of the cost: 3.7 times $1.4 billion is $5.1 billion per year. Accounting for expected cost growth, that’s a $49 billion difference over 10 years. If plans respond to the incentive, the spending will be higher. That’s a heck of a stocking stuffer.
Do you remember when the President stood firm against withering opposition last year and rallied his party to achieve an historic expansion of health insurance coverage while insisting that the bill be fiscally responsible and reduce the long run deficit? Sure was inspiring. If I were one of those members of Congress who did the right thing, voted for the bill and just lost my seat, I don’t think this latest example of the President’s generosity toward his adversaries would lift my holiday spirits.
Update: See this post for updated numbers based on new details of the program.