I wrote an overview post on the National Flood Insurance Program (NFIP) that is linked below; read that first. While that program is important in its own right, this week I am writing a series of posts considering what the 43 year old history of the NFIP could mean for health policy, with special emphasis on Medicare.
- Overview of National Flood Insurance Program
- NFIP and Health Policy-1: Why were NFIP and Medicare passed?
This post will compare the distribution of risk in the NFIP and the Medicare program, and consider what this means for reform of these two programs. The spending in both is highly concentrated, and the universal and mandatory nature of the programs serve to spread the costs of this concentrated risk. Spreading the risk means that those of lower risk cross-subsidize those at higher risk, though it is easier to determine which is which in the NFIP than it is in Medicare.
- In the NFIP, 1% of the insured properties incurred 38% of the flood losses from 1978-2004 according to GAO. Note this is assessed longitudinally.
- In Medicare, around 10% of the beneficiaries incurred 42% of the total costs in 2006. Note this is assessed cross-sectionally.
There are some differences in the concentration of spending in the two programs that have important implications.
- The degree of risk due to flood is fairly clear, especially given the detailed risk assessments constructed by the Army Corps of Engineers that are used to create risk bands for the purpose of setting premiums. An identifiable subset of dwellings are at extreme and repeated risk of flood, while many others have virtually no risk. Thus, most homes and businesses in the U.S. will almost certainly never flood.
- The concentration of risk figure noted above for Medicare is focused on a given year, and this phenomenon is reproduced each year. However, an individual who has very low Medicare spending one year is not guaranteed to have low use the next year. And because everyone dies, and health care expenditures are strongly related to age and death (they rise quickly in the last year, and especially the last few months of life), almost no Medicare beneficiary dies without first having substantial health care expenditures. The high users of medical care are not a readily identifiable group in the same way that the properties at extreme and repeated risk of flood loss are.
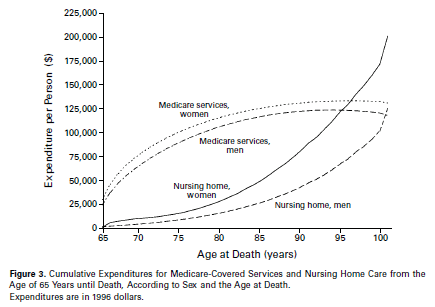
What does this mean? While both the NFIP and Medicare provide a cross-subsidy of the “sick and at risk” by the “well and not at risk”, the subsidy is more profound for flood insurance than it is for Medicare. That is because of the relative certainty of identifying who is at the highest risk of flood, and more precisely, the fact that most dwellings are at essentially no risk of flood. It is far less precise to identify who is at risk of having larger Medicare expenditures (though women systematically cost Medicare more than men, even after accounting for longevity differences). And while the well subsidize the sick in Medicare, you cannot be sure that you will not shift into the sick category tomorrow (or your parent, or your spouse, or your child some day). And most importantly, the extreme risk concentration noted in the NFIP is identified over time and the lower bound of zero risk is quite certain, while in Medicare the zero risk lower bound is virtually unheard of for someone who attains age 65 as shown by the figure below from Spillman and Lubitz (2000).
In the case of the NFIP, we need an explicit discussion of whether such an extreme cross-subsidy of dwellings in high flood risk zones is worth it (do the benefits outweigh the costs, are the distribution of same acceptable?). In particular, should subsidies of insurance premiums for properties built prior to flood risk assessments in the early 1970s continue?* The same questions about benefits, costs and distribution of same can of course be asked about Medicare. However, in the case of Medicare, if you are worried that you are not receiving enough health care and you resent cross subsidizing the sick, just wait, you may shift groups tomorrow.
*Bipartisan Policy Center deficit reduction guidance proposes ending this subsidy, see pg. 115 on document.
Update: Austin sends along this post on persistence of spending with evidence of some high users remaining high for a two-year period. This is not Medicare only but includes spending from the program. What doesn’t exist in health care is an identifiable nearly certain zero risk, and that does exist for risk of flood.