I’ve written about this before. A new study in the NEJM does little to change my mind:
BACKGROUND
In October 2008, the Centers for Medicare and Medicaid Services (CMS) discontinued additional payments for certain hospital-acquired conditions that were deemed preventable. The effect of this policy on rates of health care–associated infections is unknown.
METHODS
Using a quasi-experimental design with interrupted time series with comparison series, we examined changes in trends of two health care–associated infections that were targeted by the CMS policy (central catheter–associated bloodstream infections and catheter-associated urinary tract infections) as compared with an outcome that was not targeted by the policy (ventilator-associated pneumonia). Hospitals participating in the National Healthcare Safety Network and reporting data on at least one health care–associated infection before the onset of the policy were eligible to participate. Data from January 2006 through March 2011 were included. We used regression models to measure the effect of the policy on changes in infection rates, adjusting for baseline trends.
The government is tired of paying for stuff that’s preventable and, perhaps, the fault of the hospitals caring for patients. So they set up a new policy that said they would no longer pay for extra care that resulted from a preventable hospital-acquired condition. Researchers set out to see how the incidence of those types of conditions were affected by this policy, compared to conditions not related to the policy. And what did they find?
RESULTS
A total of 398 hospitals or health systems contributed 14,817 to 28,339 hospital unit–months, depending on the type of infection. We observed decreasing secular trends for both targeted and nontargeted infections long before the policy was implemented. There were no significant changes in quarterly rates of central catheter–associated bloodstream infections (incidence-rate ratio in the postimplementation vs. preimplementation period, 1.00; P=0.97), catheter-associated urinary tract infections (incidence-rate ratio, 1.03; P=0.08), or ventilator-associated pneumonia (incidence-rate ratio, 0.99; P=0.52) after the policy implementation. Our findings did not differ for hospitals in states without mandatory reporting, nor did it differ according to the quartile of percentage of Medicare admissions or hospital size, type of ownership, or teaching status.
CONCLUSIONS
We found no evidence that the 2008 CMS policy to reduce payments for central catheter–associated bloodstream infections and catheter-associated urinary tract infections had any measurable effect on infection rates in U.S. hospitals. (Funded by the Agency for Healthcare Research and Quality.)
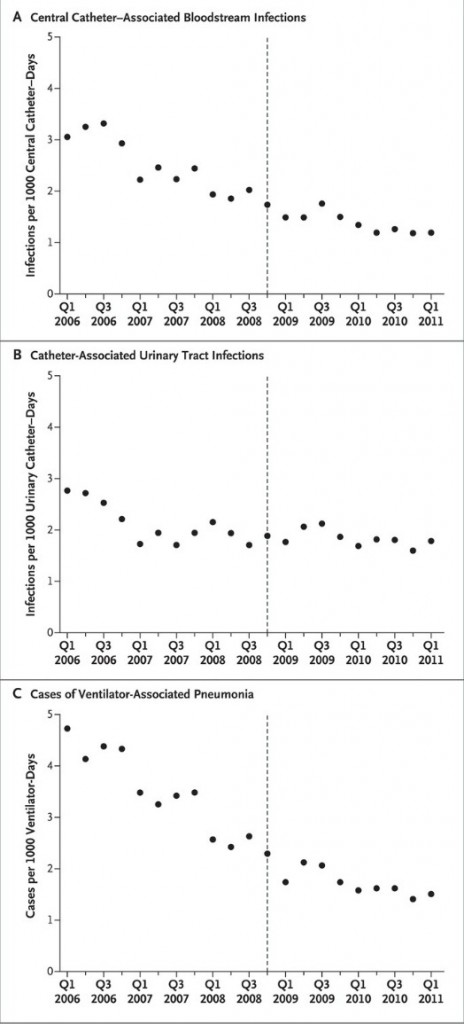
Look, the good news is that even before the policy went into place, these hospitals were working to reduce the rates of infections. They were succeeding! Starting in the fourth quarter of 2008, though, when the policy went into effect, no more significant changes were seen in the quarterly rates of these infections. Here’s the money shot:
It’s not that I don’t think hospitals can’t improve, or that I don’t think this stuff isn’t important. I just think that the ways we often go about trying to pay for performance are ineffective.
By the way, this research was funded by the Agency for Healthcare Research and Quality. I’m just saying.