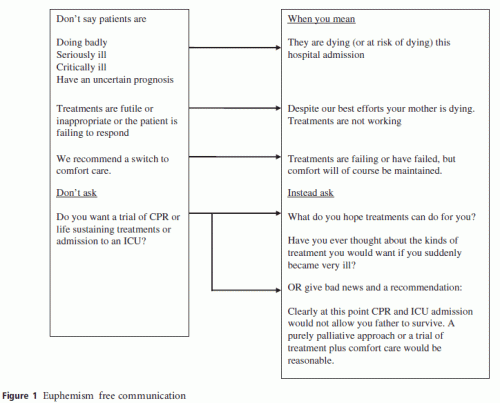
Paula Span in The New Old Age blog in the New York times has an interesting question-and-answer with Dr. Stephen Workman, an internist from Halifax, Nova Scotia, discussing communication with dying patients, based on some of his recent work. The essence of his communication recommendations are captured is this flow chart:
Go and read the entire interview. This quote summed up Dr. Workman’s approach to deal with his own patients:
Q. You specifically say someone is dying?
A. If death is such a terrible thing that I, the doctor, am unable to face it, then I’m asking too much. If I can’t talk openly about dying, how can my patients and their families bridge that gap?
**********
S.R. Workman. Never say die?–as treatments fail doctors’ words must not. The International Journal of Clinical Practice 2011;65,2,117-19.
update: modified language for clarity.