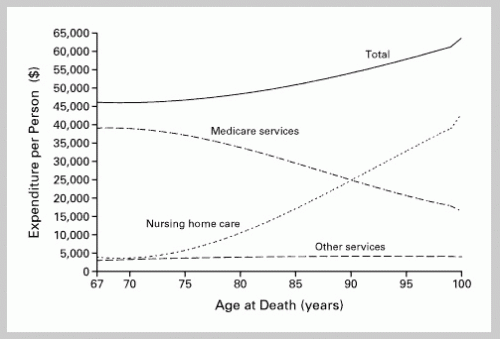
Several people have asked for more basic information about health care costs at the end of life which I will provide over several posts. Brenda Spillman and James Lubitz have done some of the classic work (a bit dated, but a model for clarity) on the relationship between age at death and cost. The first figure shows the relationship between age at death and costs in the last 2 years of life (1996 dollars). Basically, Medicare costs get lower the older a person experiences death, while nursing home costs get higher, with total costs rising with older age at death.
Note the time frame is last 2 years of life, so is more telescoped forward from death than many end of life studies, but the retrospective nature of the identification is the same.
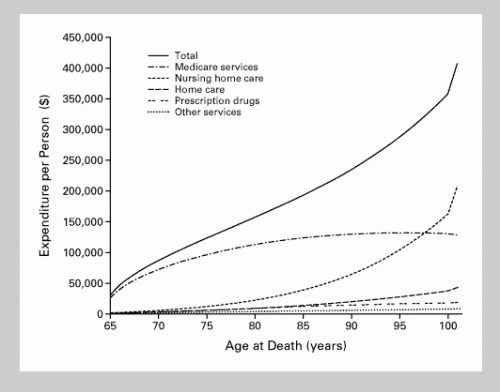
The second figure shows cumulative costs from age 65 until death, by age at death (1996 dollars). Of course cumulative costs rise with older age at death since persons were at “risk” of health care expenditures for a longer period of time. Cumulative costs are slightly higher for women than men by age of death (fig. 3 in the paper; not shown here) which is an effect separate from a gender-specific survival difference. The authors speculate this to be because diseases progress to death faster in men than women, and it is likely exacerbated by the increased chance that a wife outlives her husband.
These are high level descriptions of the relationship between cost and the age at death. The increase in nursing home costs in the two years prior to death with older death age is easy to explain; older age leads to increased disability and an increased chance of outliving your spouse which increases the risk of institutionalization.
The decrease in the Medicare cost the last 2 years of life with older age at death is a bit trickier to explain. This phenomenon coexists with the general finding that 1 in 4 Medicare dollars are spent in the last year of someones life; but the declining Medicare cost in the last two years of life with older age at death suggests there is a moderation of expenditure the older a person gets. In other words, if this phenomenon didn’t exist, the accumulation of costs relatively near death would be even greater in the Medicare program.
What cannot be answered by analyses such as this one (or really any claims based approach) are whether such decreases in the propensity to spend with older age at death are driven by explicit wishes of patients, or more implicit decisions/interactions between patients, family members and providers throughout the health care system. These are key questions.
**********
Brenda C. Spillman and James Lubitz. New England Journal of Medicine 2000; 342:1409-1415