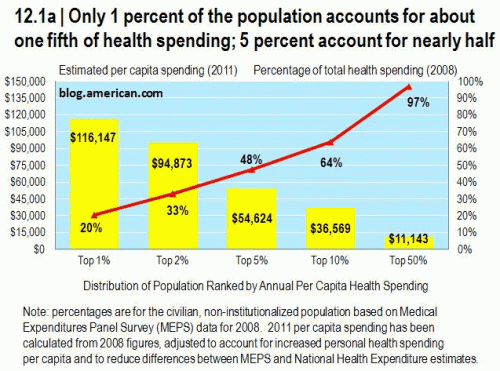
Andrew Sullivan picks up Chris Conover’s post on the other 1%–health care costs–where 1% of the population accounts for 20% of the spending.
Andrew asks:
I wonder how much of the cost for the top 1 percent in costs is spent in the last few days or weeks of life?
Focusing on Medicare, which insured around 8 in 10 persons who died last year, the proportion of total Medicare expenditures in the last year of life has been fairly stable at around 1 in 4 dollars for 3-4 decades. From a recent Annals of Internal Medicine paper by Amy Kelley and others, a focus on the last 6 months of life shows:
Median total Medicare expenditures in the last 6 months of life, adjusted to 2006 U.S. dollars, were $22 407 (range, $0 to $391 773; interquartile
range, $9087 to $40 802).
While difficult to directly compare all these numbers, the 1% identified by Conover could be thought of as the sickest subset of a very sick subset that is heavily focused in the Medicare population. Seeking to reduce end of life spending in the Medicare population seems like an obvious place to start in order to address our health care cost problems, but I have termed such savings the Fools Gold of health reform:
It is doubtful that a focus on reducing EOL spending per se will result in as much savings as is often assumed, for one simple reason: The concept of the last year of life is inherently retrospective. You do not know when the last year of someone’s life started until it ends. The stylized fact that leads to the assumption of wasteful EOL spending., i.e., 1 in 4 dollars spent on care in the last year of life, is based on an inherently retrospective concept that does not translate easily into the prospective decision-making that would be needed to reduce wasteful, futile or harmful spending in the last year of life.
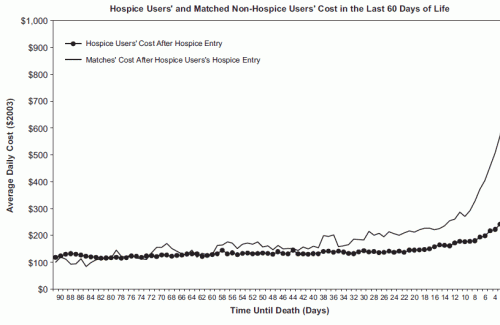
This doesn’t mean there is nothing that can be done. In fact, I have shown with colleagues that hospice reduces Medicare costs by around $2,300 from the point of hospice initiation as compared to what costs would have been without hospice (a 6-7% reduction in last year of life costs in our sample). The biggest daily savings due to hospice come in the last few days of life (see figure below) when hospice users avoid hospitalizations that are typically common near death, and maximum savings were realized in our study with a hospice stay of around 8 weeks (median hospice stays are today around 16 days). Thus, around 7 in 10 persons using hospice would reduce Medicare expenditures by using hospice for longer before death, and a little over 4 in 10 Medicare decedents now use hospice prior to death (see page 266 of this report).
There are things we can do to reduce costs at the end of life like seeking to expand hospice use, but we likely need a more systematic way of asking whether care is “worth it” throughout the system in order to develop a sustainable health care system. Only focusing on end of life spending will likely disappoint because doing so will require us to determine when people are near death AND to then change how they are treated. The technical problems are hard enough, but the cultural and political ones inherent in this strategy are enormous. I expand in great detail on these issues and my view that our nation has a cultural fear of death that enables the politics of health care cost control and rationing to be so potent in my book (ch. 3-6). We need to try everything, but I think that focusing on end of life spending as a cost control strategy is unlikely to be a panacea for our cost problem.
*******
Amy S. Kelley, MD, MSHS; Susan L. Ettner, PhD; R. Sean Morrison, MD; Qingling Du, MS; Neil S. Wenger, MD, MPH; and Catherine A. Sarkisian, MD, MSHS. Determinants of Medical Expenditures in the Last 6 Months of Life. Ann Intern Med. 2011;154:235-242.
Donald H. Taylor, Jr. Jan Ostermann, Courtney Harold Van Houtwen, Karen A. Steinhauser, James Tulsky. What Length of Hospice Use Maximizes Expenditure Savings: Evidence from the U.S. Medicare Program. Social Science and Medicine 2007;65:1466-78.
Kathleen T. Unroe et al. Resource Use in the Last 6 Months of Life Among Medicare Beneficiaries with Heart Failure, 2000-07. Arch Intern Med 2011:171(3):196-203.