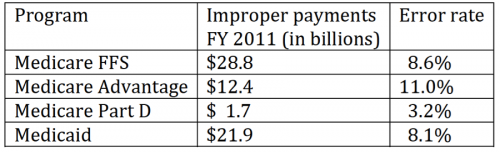
Medicare and Medicaid have active fraud detection units that are setting records for recoveries. The HHS effort is not entirely in-house, but also partners with insurance companies and other stakeholders to detect fraud. And yet the programs suffer billions in “improper payments:”
Source: GAO 2012
We need some fresh ideas. Perhaps we could use crowd sourcing, like the work that Charles Ornstein at ProPublica is doing with Medicare biller data that was recently made public:
On Friday, I emailed you my story about how a misdirected fanny pack unraveled a Medicare fraud scheme.
I’m back today with another story that was buried in Medicare’s doctor data dump, about why Illinois leads the nation in group psychotherapy sessions for patients. I found three ob/gyns and a thoracic surgeon who were paid for more than 37,000 psychotherapy sessions in 2012—more than all providers in the state of California COMBINED…
The billings for group psychotherapy reveal other unusual patterns. A Queens, N.Y., primary care doctor, Mark Burke, was paid for more sessions than anyone else in the country — 20,841. He accounted for nearly one in every six sessions delivered in the entire state of New York in Medicare, separate data show. He did not return messages left at his office.
Another large biller was Makeba Gordon, a social worker in Detroit. She was reimbursed for nearly 5,000 group therapy sessions for her 26 Medicare patients, an average of 190 each. She also billed for 2,820 individual psychotherapy visits for the same 26 patients, who allegedly would have received an average of 298 therapy sessions apiece in 2012. Gordon could not be reached for comment. [see the Chicago Tribune].
If we really wanted to jumpstart fraud detection, we’d give a reward for identifying cases like this. Whistleblowers can receive 25 – 33% of the settlement, but crowd sourcing (and investigative reporting like this) won’t qualify because the key data was public, hidden in plain sight.
UPDATE: The FY 2013 improper payments numbers didn’t report Medicare Part D, but note how the estimates vary over time:
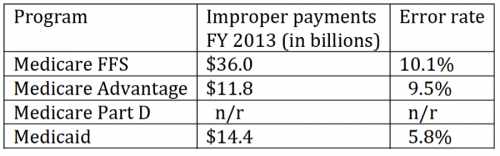 Source: GAO 2014
Source: GAO 2014
UPDATE 2: Good points from twitter & email:
@koutterson