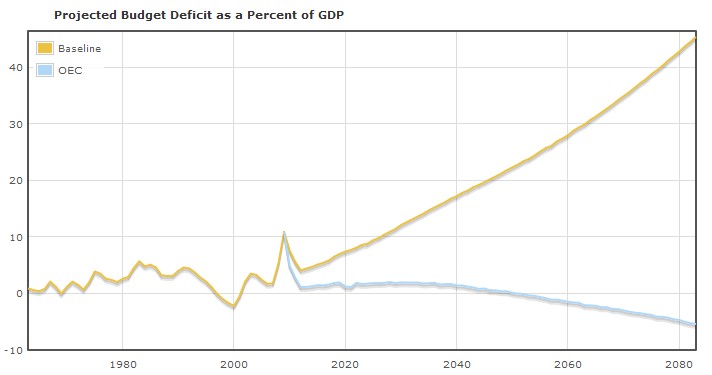
The hat trick goes to Ezra Klein for posting a great graph (a version of which is below), saying something sensible about it (quoted below), and bringing to my attention the graph’s source: the Health Care Budget Deficit Calculator, produced by the Center for Economic and Policy Research. The following graph is just one of many users can produce in a few clicks with the calculator. It shows the effect on the U.S. budget deficit as percent of GDP of a continuation of baseline health care cost trends (yellow line) and of a change to health cost trends of high income OECD countries (blue line).
As I and many other sensible observers of our health care system and its costs have said before, the health reforms that may pass this weekend won’t mark the end of our struggle with health care costs. At best they are just a beginning.
About this, and the graph, Klein writes,
Our long-term deficit is not a function of our current spending, which is manageable. It is a function of our expected spending growth, particularly in health care. With the system growing at 8 percent a year and GDP growing at 2 percent or 3 percent a year, there’s a real long-term problem there. But you can’t cut, or even tax, your way out of it. If you cut 5 percent from the system in one year, that cut disappears by the next year.
The fundamental problem here is the ratio between GDP growth and spending growth. If the two are in line, we can keep up. If not, we can’t. The only solutions that will work in the long term will be those that either increase our rate of GDP growth or decrease our rate of spending growth. That’s why I like to say that after we pass health-care reform, we’re going to need to pass health-care reform. Unless you can bring the sector’s growth under control, there’s no way to get the deficit under control.
But if you can bring our costs more in line with international norms, the deficit problem disappears entirely.
The health care cost problem is the deficit problem. It makes no sense to argue for a focus on one without the other. Reasonable people can disagree about how to control health care costs but not whether health care cost control is the route to deficit control. But we can only disagree about any of this for so long. At some point we have to actually do something. Maybe, come Monday, we will have finally started to do so.