Earlier, I posted some slides on why I’m skeptical that health savings accounts and cost-sharing won’t work like some hope because those who spend by far the most won’t be influenced by them. I’d like to take some time exploring those people who are high spenders. Remember – the top 5% of spenders account for about half of all personal health spending. Who are they?
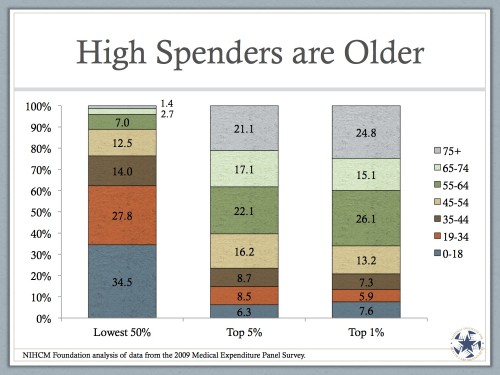
Who likes HSA’s the most? Young, healthy people (check out Figure 4). They’re in the left column. Look at the middle column, though. Americans below the age of 45 make up only 23.5% of the big spenders. Moreover, 38.2% of the big spenders are on Medicare – and none of this reallyapplies to them anyway.
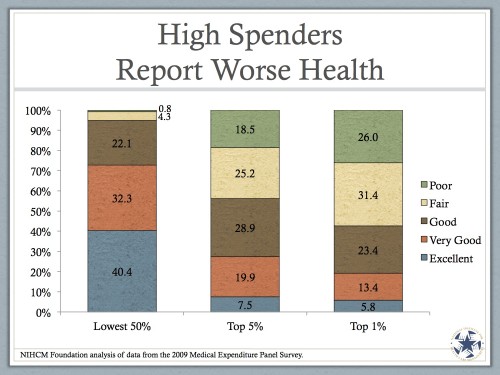
As you can see in the left column, the bottom 50% of spenders (who account for less than 3% of all personal health spending) are primarily in good, very good, or excellent health. Only about 5% of them are in poor or fair health. Compare that to the top 5% of spenders. More than 43% of them are in poor or fair health. They’re sick. They not only won’t spend less, I’m not even sure they should spend less. They’re not in good health!
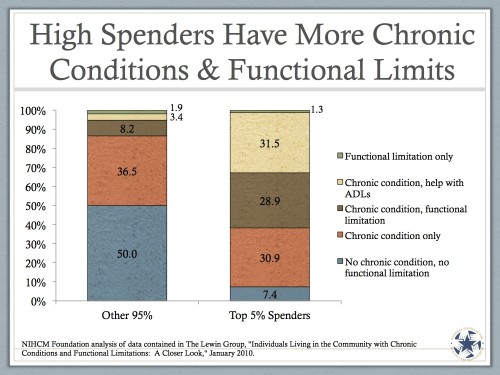
One more chart:
If we look at the bottom 95% of spenders (who account for about half of all personal health spending), about half of them have no functional limitations or chronic conditions. They’re totally healthy. Only 7.4% of the top 5% of spenders can claim the same. Almost all of the big spenders have a chronic condition, have a chronic condition and a functional limitation, or have a chronic condition and need help with activities of daily life. They are sick, and need help. And they will (and likely should) spend money to get it.
Health savings accounts, and increased cost sharing, will likely work for those who don’t need the care and are healthy. But they spend so little, that even if they are influenced, we won’t save much. Those who are spending the real money are older, sicker, and need help. If they spend less, it’s more likely they will suffer. And it’s likely many won’t spend less, since there’s no chance of their keeping money in their accounts. If they don’t spend less, then we can’t save real money.
I get why people think cost sharing and HSAs will work. But when the theoretical possibilities meet the real demographics and patterns of spending, I can’t see how this will work.