I have written about my worries that exclusion criteria for randomized control trials (RCT) limit their representativeness. Similarly, I have been worried about the “optics” of the ongoing statin discontinuation trial for persons with low life expectancy that is described in that linked post. When I have discussed this RCT on the effects of removing statins from those with very short life expectancy, many have said “why are you doing that study? Just stop giving them those medicines, they are a waste of money.”
A new paper in JAMA shows why this study needs to be done. Patients who are admitted to the hospital, and especially those who are in intensive care units, are much more likely to experience unintentional discontinuation of prescription drugs with some bad outcomes linked to such omissions. This study compared three patient groups using all hospitalizations in Ontario, Canada from1997-2009 using administrative data:
We identified 3 distinct cohorts: (1) patients who were discharged after a hospitalization that included an ICU admission; (2) patients who were discharged after a hospitalization that did not include an ICU admission; and (3) patients who were not hospitalized (controls). Patients who died during hospitalization were excluded. These 3 patient cohorts were assessed for the outcome of failure to renew the prescription within 90 days after hospital discharge
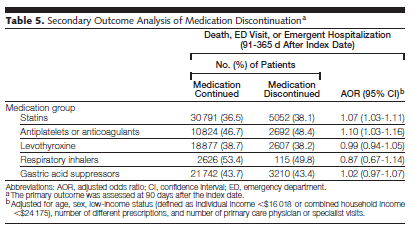
The paper provides a detailed assessment of the risk factors for failing to continue a prescription that should have been continued. However, what caught my eye were the negative secondary outcomes associated with stopping a prescription (Death, ED visit, emergent hospitalization from 3 – 12 months after index hospitalization).
This is an observational study, so you cannot be sure that whatever caused patients to stop taking their medicine wasn’t also independently related to these negative outcomes, though they did control for many factors. Those who discontinued statins were around 7 percent more likely to have one of these negative outcomes as compared to those who continued their statin (OR 1.07, 95% CI 1.03-1.11). Very ill patients with low life expectancy could be particularly vulnerable to how changes in pharmaceuticals could impact their health, quality of life, cost and mortality. This study demonstrates that that we need more evidence base even in stopping medicines among persons who are quite ill, because the potential side effects could have many negative impacts.