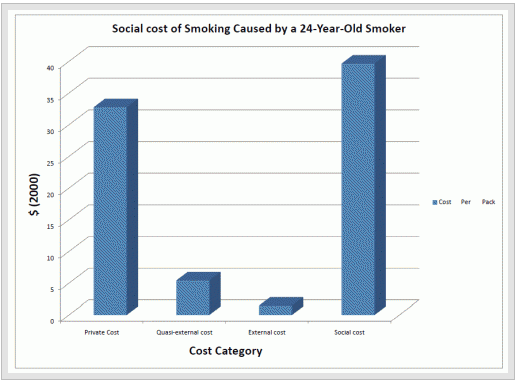
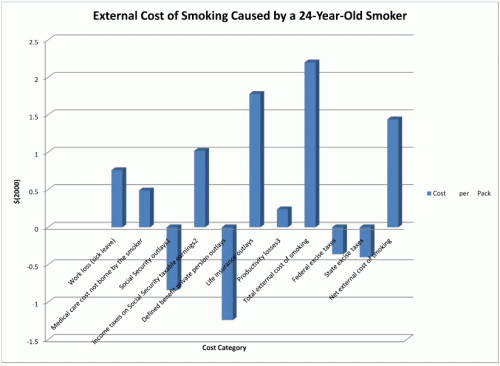
This is the fourth and final post on the social cost of smoking, which is estimated to be $40/pack. Prior posts have focused on the private cost ($33/pack), or those costs borne by smokers themselves, and the quasi-external costs ($5.50/pack), or those costs that were imposed upon the family of smokers. This post focuses on external costs, or those imposed on society by smoking. They are relatively small, around $1.50/pack, but may be the most important component of the social cost of smoking from a public policy perspective, because they represent a private action imposing costs on society.
Our cost estimation method compared the costs experienced by 24 year old smokers in 2000 with non smokers, and calculated life cycle estimates of cost that accounted for smoking cessation as well as differential morbidity and mortality that were related to smoking. To do this we identified the magnitude of specific external costs and then subtracted the excise taxes paid by smokers to arrive at the net external cost. We projected that the average excise taxes paid by 24 year old smokers in the year 2000 over the course of their smoking career would be $0.36/pack in federal taxes and $0.40/pack in state taxes. Our estimates were based on national averages in 2000 and were not done in a state-specific manner. In sum, our results show that while smokers could be expected to pay around $0.76/pack in excise taxes, the costs their smoking imposes on society is higher. This yields our net external cost estimate of around $1.50/pack.
Major sources of external cost include life insurance outlays of $1.78/pack. This figure means that smokers (who do pay higher life insurance premiums) do not pay premiums that are high enough to account for their observed mortality as compared to non smokers who purchase private life insurance. This is an example of private decisions on the part of smokers and non smokers in life insurance markets that have the effect of non smokers cross subsidizing smokers. The magnitude of the effect is larger than the net external costs of smoking. Other external costs include foregone tax receipts on lost Social Security taxable earnings ($1.02/pack), work loss due to sick leave, ($0.76/pack), and small productivity losses while smokers do work ($0.24/pack), again as compared to non smokers.
Across the entire smoking career, smokers impose around $0.49/pack in external medical care costs that are not borne by the smoker. However, the impact differs substantially by the type of payer. Private insurers bear the majority of the brunt, with Medicaid experiencing smaller increased costs due to smoking. However, smokers have lower Medicare costs relative to non smokers when using our life cycle cost estimation approach. The increased cost of smoking to private insurance, and smaller increases to Medicaid due to smoking are simply larger than the reduction in lifetime Medicare benefits that smokers receive.
Smokers also cross subsidize non smokers in both public and private retirement plans (pay in more than they take out compared to non smokers). Social Security outlays are $0.82/pack lower for smokers, due to the greatly shortened life span that they experience (net of increased Social Security disability payments). Smokers similarly cross subsidize non smokers in private pension plans to the tune of $1.24/pack.
The present value of the external costs imposed on society by a 24 year old smoker in 2000 was $6,201 ($3,829 for female smokers and $8,001 for male smokers). The total national external cost estimate for the cohort of 24 year old smokers in 2000 was around $7.5 Billion. As with the other types of costs, this is an incidence estimate, so each successive cohort of 24 year old smokers would impose external costs of similar magnitude upon society.
When assessing external costs, a key public policy question is ‘are cigarette taxes too low, or too high?’ When we wrote this book (analyses were completed in 2002), the external costs of smoking were around $1.50/pack, which leads to a public policy conclusion that excise taxes were too low and should be raised. Since then, such taxes (federal and state) have risen dramatically. The weighted average excise taxes paid per pack we used to identify the net external cost was $0.76/pack; a recent RWJF study provides a national average excise tax of $2.13/pack at the end of 2009 (2009 saw a sharp increase in the federal tax to $1.01/pack; state taxes have gradually risen and the national weighted average in 2009 was $1.12/pack). While there is little reason to believe there have been large changes in the private and quasi-external cost of smoking since we finished the book, there is good reason to believe that the aggregate level of tobacco excise taxes collected now are now very close to the pure external costs imposed by smoking. It is important to remember that the tax estimate we used in 2002 as well as the one provided by the RWJF study, represent average state excise taxes, when in fact actual tax rates differ dramatically by state; these state-level cross subsidies were not accounted for in our study. Further,even some localities have imposed large excise taxes, such as New York City which now has a $1.50 tax, and Cook County, Il. that has a $3.00/pack excise tax (all of these are in addition to state and federal taxes).
Several points to highlight:
- It is likely that cigarette taxes are near the external cost level at current rates of taxation. If the goal is for tobacco taxes to simply account for the purely external costs of smoking, then that policy goal has roughly been achieved. However, we have identified a substantial quasi-external cost burden of smoking ($5.50/pack) which is far above the current average excise tax rates in the U.S. If these costs are indeed viewed as external, then excise taxes remain far too low.
- There are other public policy reasons to further increase tobacco taxes, namely seeking to reduce smoking and simply to raise revenue. Increases in the price of cigarettes (see p. 11, Fig. 2 of the RWJF report) are linked with both reduced uptake of smoking as well as with increased cessation. Further tax increases could be justified as a smoking cessation policy as well as a smoking prevention policy. The view of smoking as purely private action is argued against because of both the addictive nature of the product as well as harm that is imposed upon children who cannot choose. Gruber and Koszegi, (2001) and Gruber and Mullainathan (2002) argue that excise taxes are a ‘smoker self control device’ designed to lessen individual harm, primarily in the form of shortened lifespan. If this view is taken, then excise taxes are far too low given how high the private costs of smoking are found to be. So, excise taxes are likely to continue to increase. Whatever the motivation for setting tax rates at a given level, a key policy issue will remain the degree to which these monies are used for cessation and prevention as opposed to being used by states to simply raise revenue for general purposes.
- Smokers cross subsidize Social Security, as well as Medicare, meaning smokers receive less in benefits paid out, even after accounting for the fact that they pay in slightly less as compared to non smokers. If you play the thought experiment ‘what if no one smoked’ then one answer is that the financing problems of Social Security and Medicare would be worse than they are today. The primary reason is the large impact of smoking on mortality. In the smoking life table that underlies this project, of 100,000 24 year old male smokers, only 74,618 would be expected to survive to age 65 if their cessation rates followed population averages for four decades. The number of 24 year old never smokers expected to survive to age 65 out of 100,000 is 87,480. Thus, around 13% more 24 year old smokers than 24 year old never smokers will pay into Social Security and Medicare, albeit at slightly reduced rates, but die before they reach the age of typical eligibility for benefits.
- The magnitude of this effect is larger for Social Security than it is for Medicare because of the differences in benefits in the two programs. Social Security provides cash that is indexed to inflation, while Medicare pays for health care whose costs are rising must faster than inflation. To give a sense of the magnitude, male smokers receive $5,264 less than non smokers from Social Security, and $2,763 less in lifetime Medicare benefits than non smokers. In Social Security, smokers just get benefits for a shorter period, on average. In Medicare, they get benefits for a shorter period, but are more expensive than average while doing so. The accounting cross subsidies pointed out are facts that we have identified using a life cycle cost estimation strategy; they do not imply that reducing mortality from smoking is not a public policy priority. If you analyzed Medicare beneficiaries at a point in time you would find their costs were higher than non smokers and could conclude that smoking increases costs, which they certainly do in a cross sectional, or prevalence perspective. It is just that such an approach masks the profound mortality burden that smoking exhibits on cohorts of persons before they even attain Medicare eligibility. How important seeking to end the huge private cost that is imposed by smoking on smokers through a shortened life is a value judgment.
- Smoking increases overall health care costs in spite of reducing Medicare outlays; private insurers bear the brunt of these increased costs. For male smokers, private insurers experience over $5,000 in increased costs, while Medicaid has costs increased by around $300. For women the corresponding figures are $3,000 and $1,300. There are a variety of states considering policies to either increase premiums or cost share amounts for smokers covered by Medicaid or State Employee insurance programs. Our estimates show that private insurance companies could be seen as justified in adding such surcharges. A key question is whether such charges are simply designed to require smokers to self finance their extra costs while covered by private insurance, or if the goal is to finance expanded cessation programs? The former would be adopting a prevalence perspective on smoking, but for private insurers who may cover someone this year but not next, that is the perspective that makes business sense. For Medicaid, the smoking cost differentials are smaller, and it is more difficult to interpret what they mean since Medicaid provides both acute care coverage in addition to being the primary payer of nursing home care services for the elderly. Again, the key question for states considering Medicaid smoking surcharges is what is the goal of the policy?
Over the summer I will be writing some follow up posts to this series that focus on different aspects of the smoking issue, and which discuss broader applications of the life cycle cost estimation strategy approach that we used. Look for around one/week.
Full citation: Frank A. Sloan, Jan Ostermann, Gabriel Picone, Christopher Conover and Donald H. Taylor, Jr. The Price of Smoking. MIT Press: 2004. The Price of Smoking is available as an ebook.
J. Gruber and B. Koszegi (2001). Is Addiction Rational? Theory and Evidence. Quarterly Journal of Economics 116:1261-1303.
J. Gruber and S. Mullainathan (2002). Do Cigarette Taxes Make Smokers Happier? Cambridge, MA: NBER working paper #8872.