Continuing upon my post last week making the point that Medicaid is really 3 distinct programs:
- Program 1: covers mainly pregnant women and children for acute services. There are around 45 Million such persons. The ACA would expand this portion of the the program greatly. This is the group that experienced barriers to access in the recent study, and this is where most of the debate is centered. Such beneficiaries are numerous, but are relatively inexpensive on a per capita basis.
- Program 2: covers long term care, most notably nursing home care for Medicare beneficiaries who are also poor and therefore covered by Medicaid. Such persons are know as Dual Eligibles, because they are covered by both Medicare and Medicaid). There are 9 Million duals, around two-thirds of them are eligible for Medicare because of age, the remainder due to permanent disability. This relatively small number of persons are extremely costly to both Medicare and Medicaid.
- Program 3: covers long term care and acute specialized services for persons younger than 65 who are disabled, but not eligible for Medicare; There are 5.9 Million such persons, who are more difficult to describe because of their variety of needs.
Most policy attention is paid to the reform of Program 1 above. This post focuses on reform of the most expensive aspect of the Medicaid program—long term care—which is the primary concern of Program 2 (dual eligibles) and Program 3 (disabled persons younger than 65 not eligible for Medicare) above. A key policy question is where should services be provided to elderly and disabled Medicaid beneficiaries? Charles Milligan and Cynthia Woodcock addressed this issue during their presentation “Rebalancing Long-Term Services and Supports: Progress to Date and a Research Agenda for the Future” at AcademyHealth’s Annual Meeting Long Term Care Colloquium last week in Seattle.
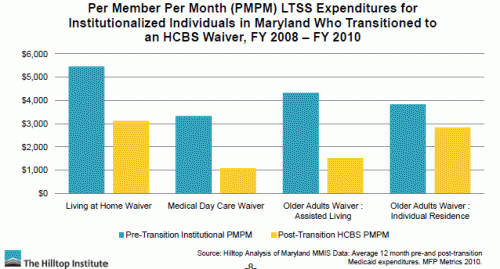
Around 75 LTC researchers and policy makers attended this 3-hour session (presentation of paper, discussants and general discussion) that focused on the desirability of “rebalancing” LTC services away from institutions (esp Nursing Homes) and toward home and community based services (HCBS). Milligan and Woodcock show evidence from Medicaid waiver programs in the State of Maryland documenting reductions in per member, per month Medicaid costs when moving persons from institutions to community-based settings via waiver programs that typically allow for the provision of non-standard benefits for persons covered by Medicaid.
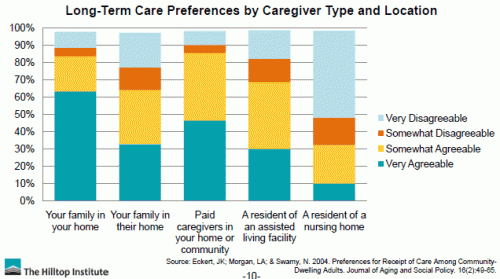
What is missing from this assessment is the outcome, or quality of services provided. The need to better link different service models with outcomes was roundly noted as a tremendous research and policy need. However, from a preference perspective, patients are far more favorable to community based, as compared to institutional settings, which is no surprise.
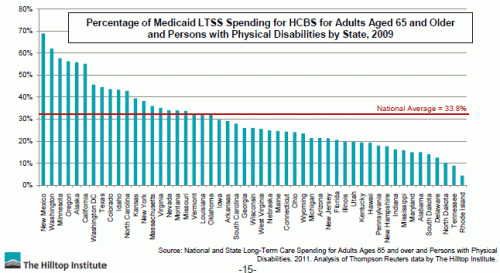
There has been steady movement from institutional toward HCBS in Medicaid over the past decade and a half. In 1997, around 75% of total Medicaid long term care expenditures were for institutional care (mostly nursing homes), while it had dropped to around 66% in 2009; the remainder of the LTC was delivered in HCBS. The are very large state differences in how Medicaid programs have spent long term care dollars, which would make clearer linkages with outcomes even more potentially informative. For example, New Mexico is now spending around 7 in 10 Medicaid LTC dollars spent on dual eligible and disabled persons on HCBS; at the other end of the spectrum, Rhode Island and Tennessee are spending less than 1 in 10 Medicaid LTC dollars on HCBS.
The most interesting aspect of the discussion following Milligan and Woodcock’s excellent presentation and the formal discussant remarks was the degree of pushback from the audience against the notion that it is self evident that rebalancing away from institutional toward HCBS is always the best policy. There was a general refrain of ‘it depends, we need to know more.’
In particular, there were concerns that we do not know as much as we should about the relative outcomes of particular sites/types of care provided to disabled Medicaid beneficiaries, be they dual eligibles or persons included in “program 3” noted above. This information is needed in a clearer fashion to be able to determine the correct mixture of institutional versus HCBS in Medicaid-financed LTC. The need to determine the appropriate setting for long term care services (institutional v. home and community based) will intensify, as the movement of the baby boomers into retirement years and the fact that the national nursing facility occupancy rate is around 85% (according to the commissioned paper by Milligan and Woodcock that is not yet publicly available). The figures shown above include dual eligibles (program 2 above) and disabled persons who were not also eligible for Medicare (program 3).
A few thoughts about Medicaid reform in light of this conference and discussion:
- A classic Medicaid worry around developing community-based services (not Nursing homes) is the wood work effect, meaning that persons will be more likely to seek eligibility and to use services if they do not have to reside in a nursing home to do so. Such an effect could offset the reduced per capita cost of non institutional settings. Whether there were a net increase or decrease in overall costs is ambiguous, and would depend upon the degree of woodwork effect and per capita savings as compared to placement in a nursing home.
- A further Medicaid worry is back fill in nursing homes, meaning as you transition patients out of nursing homes to HCBS, will other patients simply end up in nursing homes, on the route to spend down to Medicaid eligibility?
- The potential woodwork effect would seem to be a bigger issue with program 3 above, in part because the population at risk and in need of services is harder to define. We don’t know how many people need such services, while the number of Medicare beneficiaries who are spent down to Medicaid is clearer. Another way to describe an increase in covered persons that may be termed woodwork effect is the provision of care to those in need. An increase in beneficiaries covered by Medicaid who fall into Program 3 is consistent with both narratives.
- For program 2, the dual eligibles, the wood work effect could still exist from Medicaid’s perspective, but not from Medicare’s. Medicare is on the hook for the acute care cost of the dual eligibles no matter what, and poor quality long term care could be expected to increase those costs. Likewise, there are incentives of providers who bill Medicaid for the care of dual eligibles (like Nursing homes and bed hold payments) and the states to send patients to hospitals for non-productive care in times of high patient acuity that results in a shifting of cost from the states to the federal government. Small changes in such nursing home admissions could be expected to improve quality of life for patients in a way that held net costs constant or reduced them (on a per capita basis).
Federalizing the Medicaid/LTC costs of the dual eligibles (program 2 above) and making Medicare responsible for all of the care of the dual eligibles seem to be more clearly warranted than federalizing the care of disabled Medicaid beneficiaries who are not eligible for Medicare (Program 3 above). Making Medicare responsible for all of the care of the dual eligibles seems to provide the best hope of getting the appropriate level of care for elderly, disabled persons, many of whom are living in nursing homes. And since Medicare is already responsible for acute care services for these patients, federalizing Medicaid for dual eligibles would remove the issue of cost shifting from states to the federal government under the current situation which is almost certainly not associated with the best care for patients.
How to best reform program 3, the disabled, non-dual eligible Medicaid eligible patients is trickier, and it remains unclear to me of the best way forward to care for such persons, many of whom will need specialized care for years or even decades. I am not opposed to federalizing this portion of Medicaid, I just need to know more. I think that moving ahead to federalize Medicaid for the dual eligibles makes sense. In any event, more information is needed on the benefits, quality and cost of care provided across different LTC settings for both of these ‘programs’. Moving to federalize Medicaid for the dual eligibles would likely help produce such information since one would payer would be responsible and have a clear incentive to find the answers.