Aaron has written recently to reject notions that physicians must sacrifice all to work full time, no matter what. The discussion has focused on the role of female physicians choosing to work part time, and whether this is a legitimate choice or not. This debate reminded me of research I did during a post doc at the University of Manchester (U.K.) in 1996-97 that resulted in a paper in the BMJ in 1997 entitled, “Recruitment, retention, and time commitment change of general practitioners in England and Wales, 1990-4: a retrospective study.”
The data are 20 years old, but I think the way we framed the empirical analysis is useful. The context was the rapid increase in the proportion of English medical trainees who were women during the 1980s, and subsequent worries that the higher rate of female General Practitioners in the NHS would mean that they were not training enough GPs to produce the needed full time equivalent GPs given the movement toward part time practice.
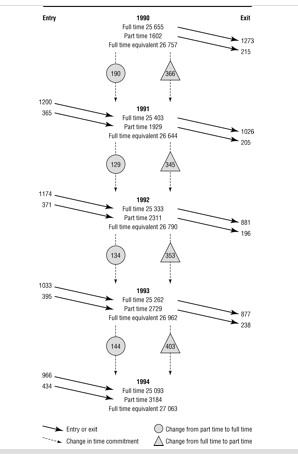
This figure showed the physics that produced GP supply available in the NHS: movement into practice, out of practice, and changes from full-to-part time and vice-versa. We were able to nail this down definitively for the entire NHS due to data sources, since virtually all GPs billed the NHS, and they had to be able to bill the NHS in order to practice (most private insurance in the UK is que-jumping, specialty insurance, and most private insurance plans provide for patients to use NHS GPs). I don’t believe you could nail down such a pretty picture of the primary care supply in the U.S. because you would have to piece it together from different sources and wouldn’t have as clear a measurement of time status (full v. part time), but this is the way to think about primary care supply (or any other provider supply).
Table 2 from the paper clearly showed the increased likelihood of female GPs to practice part time as compared to men, at younger ages (<35, 35-49), but the opposite at older ages, where male GPs were more likely to practice part time than females at 50-59 and 60 and over (note that these figures are contingent upon remaining in practice at all).
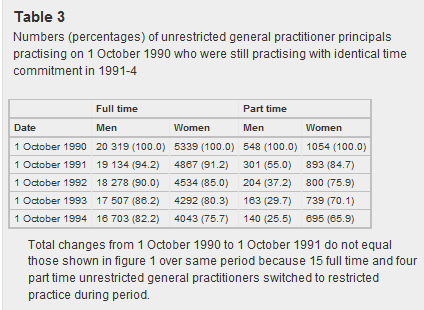
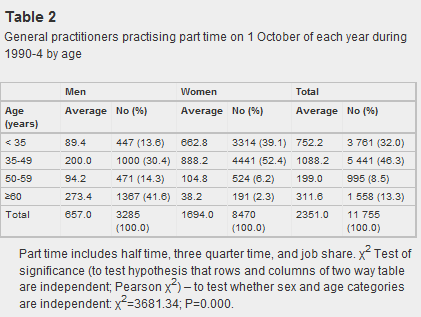 Table 3 in the paper provides a simplistic survival analysis of the stability of GPs remaining in their Oct. 1, 1990 practice status (full v. part time) for 5 years.
Table 3 in the paper provides a simplistic survival analysis of the stability of GPs remaining in their Oct. 1, 1990 practice status (full v. part time) for 5 years.
 It seems obvious to me that physicians, just like everyone else has to figure out a work/life balance that makes sense for them, and everyone will not choose the same course of action. There are gender differences in the choices, and these are simply facts that go into determining the supply of providers. While you could not produce such a clean picture of primary care or specialty care supply in the U.S. as we did of GPs in the early 1990s in the NHS, these are the types of relationships that produce the physician supply.
It seems obvious to me that physicians, just like everyone else has to figure out a work/life balance that makes sense for them, and everyone will not choose the same course of action. There are gender differences in the choices, and these are simply facts that go into determining the supply of providers. While you could not produce such a clean picture of primary care or specialty care supply in the U.S. as we did of GPs in the early 1990s in the NHS, these are the types of relationships that produce the physician supply.
- Recruitment into the workforce
- Retention in the workforce
- Movement between full and part time practice
- And the degree to which any of the changes are permanent or temporary
* Full citation: Donald H. Taylor, Jr., Brenda Leese. Recruitment, retention and time commitment change of general practitioners in England and Wales, 1990-4: a retrospective study. BMJ 1997; 314:1806-1810.