A new study in JAMA shows that patient choice may be bad for the health of some rural Medicare beneficiaries who experienced worse outcomes when treated for common serious conditions in critical access rural hospitals (those with less than 25 beds and more than 35 miles from the nearest hospital) as compared to other facilities.
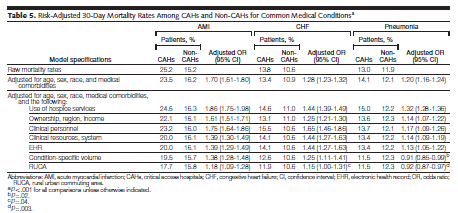
Patients treated in CAHs had higher 30 day adjusted mortality rates for AMI 23.5% v. 16.2%; CHF 13.4% v. 10.9%; pneumonia 14.1% v. 12.1%. All comparisons were statistically significant and were adjusted for age, race, sex, and medical comorbidities. These findings remain even after further controlling for selected hospital characteristics including volume, ownership, electronic medical records, and patient choices such as use of hospice. The study population was comprised of fee for service Medicare beneficiaries hospitalized nationally from 2008-09.
Choice is a powerful cultural symbol in the U.S. Fear of being denied the ability to choose where one gets care often drives anxiety about health reform. As I noted yesterday, you need to know the quality or effectiveness of care provided to be able to fully evaluate the up and downside of choice. This appears to be a case in which the unfettered choice of hospital that is afforded to Medicare beneficiaries means that patients are allowed to choose to go to hospitals with poorer outcomes. The results of the study seem fairly straightforward in this respect as the authors note in the abstract
Compared with non-CAHs, CAHs had fewer clinical capabilities, worse measured processes of care, and higher mortality rates for patients with AMI, CHF, or pneumonia.
However, it is difficult to know what we do about this? It is not a small problem, as around 1 in 5 Medicare beneficiaries receive care in CAHs. Over the next couple of days, I am going to do a series of posts more fully exploring what the results of this study mean for Medicare policy specifically, and what they tell us about the value of patient choice, more generally. Future posts will cover topics such as:
- how do CAHs differ fron non-CAHs in terms of the care they can provide?
- are there ways to improve the quality of care in such hospitals? Are there success story examples?
- methodological issues in claims-based research studies
- how important are patient preferences to receive care close to home? Are we willing to tolerate/accept worse outcomes if that is where patients want to be treated? How much worse?
- what is Medicare’s responsibility to inform patients of differences in quality among providers?
h/t Brad Flansbaum who may be blogging on this paper from the perspective of a hospitalist.
update: added a sentence about mortality findings holding up after adjustment for more covariates.