The Lancet brings the pain. “Effects of vitamin D supplements on bone mineral density: a systematic review and meta-analysis“:
Background: Findings from recent meta-analyses of vitamin D supplementation without co-administration of calcium have not shown fracture prevention, possibly because of insufficient power or inappropriate doses, or because the intervention was not targeted to deficient populations. Despite these data, almost half of older adults (older than 50 years) continue to use these supplements. Bone mineral density can be used to detect biologically significant effects in much smaller cohorts. We investigated whether vitamin D supplementation affects bone mineral density.
Methods: We searched Web of Science, Embase, and the Cochrane Database, from inception to July 8, 2012, for trials assessing the effects of vitamin D (D3 or D2, but not vitamin D metabolites) on bone mineral density. We included all randomised trials comparing interventions that differed only in vitamin D content, and which included adults (average age >20 years) without other metabolic bone diseases. We pooled data with a random effects meta-analysis with weighted mean differences and 95% CIs reported. To assess heterogeneity in results of individual studies, we used Cochran’s Q statistic and the I2 statistic. The primary endpoint was the percentage change in bone mineral density from baseline.
I’m a pediatrician, so I don’t deal with osteoporosis much. But I do deal with my friends, many of whom are convinced that supplementing individual vitamins is a great idea. That’s almost never true, unless your goal is to make really expensive urine.
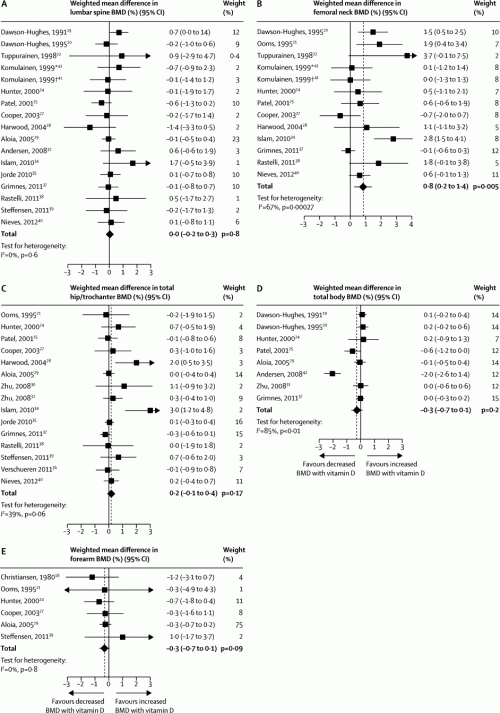
This study looked at all the medical literature studying the effect of vitamin D supplementation on bone mineral density. There were 23 studies with over 4000 participants that met inclusion criteria. Ready for the results? Six showed a benefit. Two showed a detriment. The rest showed no effect at all. They did a meta-analysis, in which they pooled all the studies together for one big analysis. Pooled odds ratio diagram below (click to enlarge):
Let me orient you here. This is showing you the odds ratio for each outcome, one study per line. If the square (and error bars) for a study are entirely to the right of the vertical line, at zero, then vitamin D was beneficial. If the square (and error bars) are entirely to the left of the line, or negative, then vitamin D was detrimental. If the square (or error bars) in any way touch the line (zero), then it’s a non-significant result. At the bottom, the results are summed into a diamond, with the same rules applying.
As you can see, there was a small benefit (weighted mean difference 0.8%) for studies looking at the efect of vitamin D supplementaion on bone mineral density (BMD) of the femoral neck. Woo. Hoo. Hip? No effect. Trochanter? No effect. Lumbar spine? No effect. Forearm? No effect.
Total body? No effect.
What do the authors of the study have to say? “Continuing widespread use of vitamin D for osteoporosis prevention in community-dwelling adults without specific risk factors for vitamin D deficiency seems to be inappropriate.”
You think?!?!?!