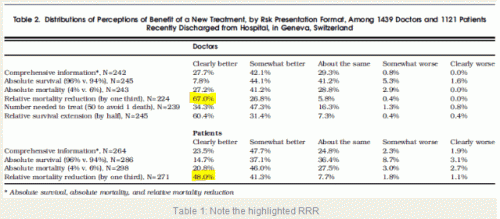
Brad Flansbaum writes about the difficulty of correctly interpreting survival odds for patients and physicians. His post is based on an interesting study about framing bias in medical decision making. He notes that physicians, in particular, may have trouble communicating small survival chances in meaningful language, and seem to systematically overstate the chances for success as compared to patients. In the paper he is citing, two-thirds of physicians attached the label “clearly better” to a reduction in relative risk of death of one-third, and absolute mortality risk reduction of 2%. Interestingly, around half of the patients in this study attached the label “clearly better” to this same risk reduction.
Brad is particularly worried about the ability of physicians to deliver information to patients in a meaningful format, which is one key component of good treatment decisions. How do we improve decision making?
I think that the best answer is more types of information to inform decisions. We need to add quality of life and cost to the mix to arrive at better decisions. Better communication about survival chances would be an improvement, but that is only part of the answer, and in and of itself won’t likely reduce costs as much as many seem to assume. Belief that better prognostication of death will lead to great cost reductions is likely the “fools gold” of health reform. We need to add information on the impact of a treatment on quality of life as well as explicitly discussing the costs of the therapy. More variables to consider, each with uncertainty, provide a more realistic setting in which to make treatment decisions. Only by learning to more directly encounter and talk about the trade-offs between survival, quality of life and cost can we hope to arrive at a reasonable answer to the bottom line questions: “is it worth it?” “should we do it?” My book has a fairly detailed discussion of these issues in chapters 3, 5 and 6.