The evidence keeps mounting that high and rising US health spending is due mostly to how intensively care is provided and the prices we pay. Disease prevalence is not the main driving force.
In recent paper in Health Affairs, Charles Roehrig and David Rousseau find that between 1996 and 2006,
increases in treated prevalence account for about one-fourth of overall growth in real per capita spending, with the remainder attributable to growth in cost per case. If cost per case had remained constant, the rate of increase in health spending would have been less than GDP growth by more than one percentage point. […]
Our evidence also suggests that most, and perhaps all, of the treated-prevalence effect is due to an increase in the share of eligible people being treated rather than an increase in clinical prevalence.
We conclude that health spending growth in excess of GDP growth is not primarily due to increases in clinical disease prevalence. Consequently, efforts to reduce future growth in disease prevalence—such as through prevention— although certainly providing many societal benefits if successful, are unlikely to reduce overall health care cost growth to levels lower than or equal to GDP growth. [Emphasis mine.]
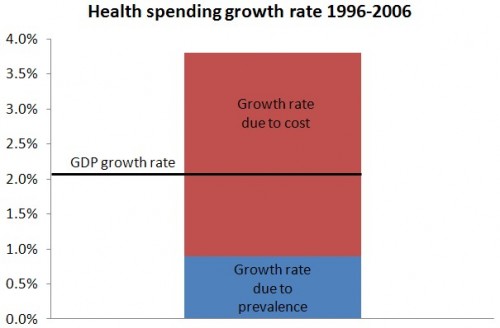
Over the period of study, the growth rate in real per capita health spending was 3.8 percent and GDP per capita grew 2.1 percent. If the cost of care had remained constant, the rate of growth due to disease prevalence alone would have been 1.1 percent. Contrast this with the conventional wisdom that holding health spending below GDP + 1 percentage point growth would be a monumental victory in cost control.
So, not only does the cost of care drive the rate of increase in health care spending, it is responsible for all of the increase in health spending above GDP growth. In fact, it is responsible for more than that. Here it is in a chart:
Some additional details:
- The authors’ analysis is based on National Health Expenditure, Medical Expenditure Panel Survey, and National Health and Nutrition Examination Survey data.
- I’ve blurred the distinction between treated prevalence and clinical prevalence (which includes those with a disease who are not treated) because the authors’ analysis shows the distinction does not matter a great deal, having no impact on the qualitative conclusions. At most, clinical prevalence contributed 0.3 percentage points to the 3.8 percent increase in real per capita spending.
- There is considerable variation by disease in the degree of contribution of prevalence to increased spending. For instance, all of the increase in spending of esophageal disorders was due to prevalence and almost none of the increase in nervous system disorders was due to prevalence.
Bottom line: prevention can’t play a major role in curbing the rate of growth in health care spending. The rationale for prevention is for health and other economic and social benefits (greater ability to work, enjoy leisure, etc.).