I’m doing a lot of reading on nutrition at the moment, and will likely get to a series on it for the blog. In the meantime, Austin alerted me to “Long term maintenance of weight loss with non-surgical interventions in obese adults: systematic review and meta-analyses of randomised controlled trials” in the BMJ:
Objective: To systematically review and describe currently available approaches to supporting maintenance of weight loss in obese adults and to assess the evidence for the effectiveness of these interventions.
Design: Systematic review with meta-analysis.
Data source:s Medline, PsycINFO, Embase, and the Cochrane Central Register of Controlled Trials.
Study selection: Studies were identified through to January 2014. Randomised trials of interventions to maintain weight loss provided to initially obese adults (aged ≥18) after weight loss of ≥5% body weight with long term (≥12 months) follow-up of weight change (main outcome) were included.
Study appraisal and synthesis: Potential studies were screened independently and in duplicate; study characteristics and outcomes were extracted. Meta-analyses were conducted to estimate the effects of interventions on weight loss maintenance with the inverse variance method and a random effects model. Results are presented as mean differences in weight change, with 95% confidence intervals.
Results: 45 trials involving 7788 individuals were included. Behavioural interventions focusing on both food intake and physical activity resulted in an average difference of −1.56 kg (95% confidence interval −2.27 to −0.86 kg; 25 comparisons, 2949 participants) in weight regain compared with controls at 12 months. Orlistat combined with behavioural interventions resulted in a −1.80 kg (−2.54 to −1.06; eight comparisons, 1738 participants) difference compared with placebo at 12 months. All orlistat studies reported higher frequencies of adverse gastrointestinal events in the experimental compared with placebo control groups. A dose-response relation for orlistat treatment was found, with 120 mg doses three times a day leading to greater weight loss maintenance (−2.34 kg, −3.03 to −1.65) compared with 60 mg and 30 mg three times a day (−0.70 kg, 95% confidence interval −1.92 to 0.52), P=0.02.
Conclusions: Behavioural interventions that deal with both diet and physical activity show small but significant benefits on weight loss maintenance.
This was a systematic review and meta-analysis of studies that examined interventions that sought to help adults maintain a weight loss of at least 5% of body weight. The good news is that interventions that focused on diet and exercise seemed to help, keeping weight “regain” 1.6 kg less than doing nothing. Using the drug orlistat also seemed to help. Woo. Hoo.
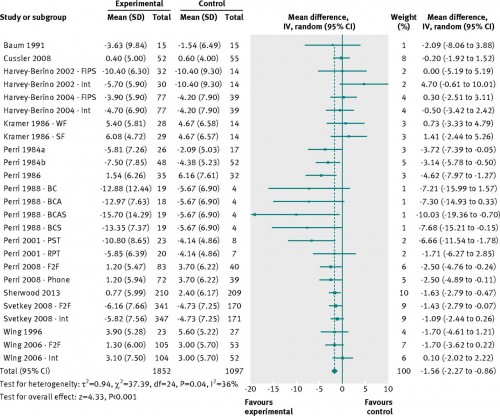
The bad news is that this is a “slowing of weight regain”. Not further weight loss. Not even maintenance of weight loss. A “slowing of weight regain”. Further, check out the figure:
These are all the studies of diet and physical activity. Any time the horizontal line crosses the vertical line at zero, the study was not significant. The pooled odds ratio (the bottom diamond) is significant and favors interventions, but so, so, so many of the studies did not. Or barely did. Keeping weight off is hard.
This part was almost comical:
There was no evidence of effectiveness for the following interventions: dietary interventions versus control condition, high carbohydrate and low fat diets versus other types of diets, physical activity interventions versus control conditions, adding aerobic exercise to a dietary intervention versus diet alone, adding physical activity (such as walking and resistance training) to a dietary intervention versus diet alone, or adding meal replacements to dietary recommendations versus dietary recommendations alone.
Other studies found no evidence for the effectiveness of nutritional supplements in addition to a dietary regimen versus the diet itself and placebo supplements or no supplements, Tapas acupressure technique versus social support, mailing computer generated individualised reports based on the “transtheoretical” model versus generic action oriented information, gourmet cooking versus neurolinguistic programming based therapy, a motivation focused versus a skill focused intervention, or providing participants with a corset over nine months versus no corset. One study reported that wearing a corset was perceived as uncomfortable—no other comments about weight loss maintenance treatments were reported.
There are times I wonder why the conclusion from studies like this isn’t “despair”.