From JAMA Internal Medicine, “Headaches and Neuroimaging. High Utilization and Costs Despite Guidelines“:
While most headaches are attributable to benign conditions, patients and physicians are often concerned about intracranial pathologic conditions. However, the yield of significant abnormalities on neuroimaging in patients with chronic headaches is 1% to 3%. Given the comparable yield in patients without headaches, multiple guidelines have recommended against routine headache neuroimaging, and efforts to improve the efficiency of health care utilization, such as the Choosing Wisely campaign (ABIM [American Board of Internal Medicine] Foundation;http://www.choosingwisely.org), have identified these tests as a target. However, little is known about recent headache neuroimaging utilization, associated expenditures, and temporal trends in the United States.
They used the National Ambulatory Medical Care Survey (NAMCS) to look at all visits for headaches from 2007 through 2010, inclusing CT and MRI scans for those visits. Care to guess what they found? Do you think that we are, perhaps, ignoring guidelines and ordering these tests?
Over a 4 year period, there were more than 51 million visits for headaches, with more than 25 million being for migraines. Neuroimaging tests, the same ones guidelines say not to get, were ordered in more than 6 million visits, and in about 2.5 million migraine visits. The costs of these tests, the ones guidelines say not to get, were about a billion dollars each year.
Oh, and lest you think we’re getting a handle on this problem, here is the trend over time:
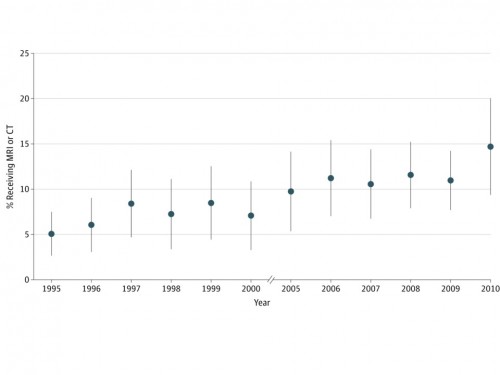
These tests are recommended by multiple agencies not to occur. They do, nonetheless. They occur to the tune of something like 1.5 million times a year at a cost of about $1 billion. You have to wonder why insurance keeps paying for them. Why don’t we just stop?

